Lipoma Excision
Transcription
CHAPTER 1
Here's the mass. It's pretty big. It feels firm. So here, I can see - I could hold it down here. See that's how long it is. And I can feel it here. So it feels like it's pretty deep. It's not that superficial. So I might have to go a little deeper, it's pretty big in there.
CHAPTER 2
Okay. Starting. 1, 2, 3.
CHAPTER 3
So I’ll start the incision. I'll start from here until here because I can feel it's a big mass. I’ll still do an elliptical incision from here. Like this. So it'll be easier for me to oppose the edges.
CHAPTER 4
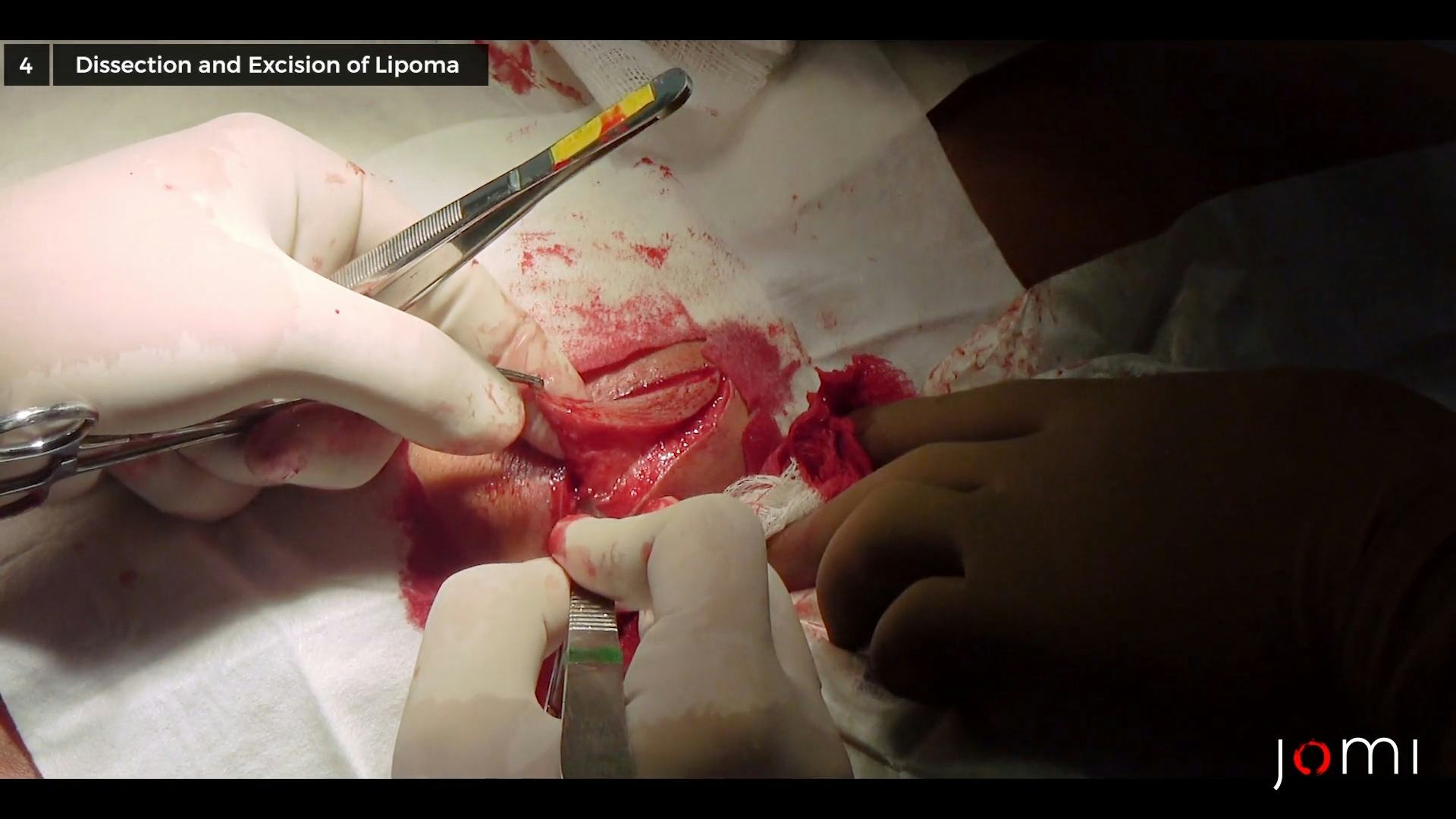
Okay. Mosquito, please. He's feeling some pain. It’s a little deep so we're going a little deeper. Just adding more anesthesia. It seems like a deep lipoma. We're already getting part of the Lipoma. It seems like a deep... Mosquito? We have some bleeders on the side, so I'm just going to clamp that. So this is a huge lipoma, underneath. We see a bit popping out already. He's had it for 8 years. It's benign, yeah. So you'll have a Mosquito here for that. So you'll have different kinds of lipomas. So this Lipoma has been here for 8 years, so it's a little more adhered to the tissues as compared to some lipomas, which are superficial and easy to remove. Once you enter its capsule, easy. But this one, since it's been here for a couple of years, sometimes it's more difficult to remove. Okay. I'm almost getting the whole thing. You can see a little popping out already. So it's important to get the plane. Once you see a plane, you just follow it, just to avoid... So I almost got - I already got the inferior part. So, here... Sometimes you can use your finger for blunt dissection. So I think we've got this portion. I'll just release this one. Mosquito. So it’s a little bloodier than the others. So I removed the lipoma.
CHAPTER 5
Mosquito. So I just apply the clamp again on that bleeder. Most likely we'll get that bleeder once we start suturing the tissues. So here you could see the defect where the mass came from. It’s pretty deep. So if I feel the edges again, it seems like we got everything. So normally, generally when it's a young patient, I would say just keeping pressure, the bleeding will stop, and, we just start closing the wound, adding internal sutures, just to control the bleeders inside.
CHAPTER 6
So I'm suturing. I'm getting internal... 3-0. Zero? 3-0. So it’s important that you get the tissues underneath, to close that cavity out. That will decrease the chances of a seroma formation. Important first to always ask the - the history of the patient, if he's taking any, any anticoagulants, any other medicines. So this is a relatively young patient - 30 - 35-year-old patient. 35. So I'm not too worried about significant postoperative bleeding. So for other patients who you think will have bleeding, it might be safe to do them in an operating room and not in an outpatient setting.
CHAPTER 7
This case would have been easier if this was done earlier. I think he waited 8 years. So it has grown significantly. And it's in an area where there's a lot of muscle, and it's a, an area where there’s lots of movement, and he also lies down in this area, so the tendency is that the lipoma, which is normally easier to remove, gets a little adherent to the soft tissues close in the muscles, so it's more difficult to remove. So it would've been better if it was earlier, but location-wise, I think it's okay, safe, no - no major vessels or structures in that area. We are hoping that - there is a chance of recurrence, but we're hoping that recurrence will not happen for this patient. 35-years-old. He had a mass, here. So we took it out, and now he's okay. He's had it for 8 years. He's Philippine Coast Guard? Philippine Coast Guard, staying here in the local island of Sibuyan, Romblon. Busy? So he's mentioning that he - he would've had it removed, but he's busy at work. So this is a good opportunity for, as missioners to go to their island, and they - they'll really be able to get good service, and go back home right away, and take care of his wounds, and recover.