Laser Stapedotomy for Otosclerosis
Transcription
CHAPTER 1
Today, this patient is a 44-year-old male who presented with progressive hearing loss in the left ear. He was seen about 5 years ago and noted to have a very mild conductive hearing loss on the left side with absent acoustic reflexes, but at that time, was not felt to be a surgical candidate yet for stapedectomy. Over 5 years, his hearing loss has progressed, and he now has about a 35 dB conductive air-bone gap in the low and mid frequencies - and he presents today for a left stapedectomy with laser. This is being done with the patient under MAC anesthesia, so he is receiving IV sedation but can be actually lightened up and awakened if we need to talk to him or to assess his hearing. All right, we are good to start prepping. So who's prepping? Are you prepping? A Betadine prep - so, a big Betadine prep, and then it's okay to squirt some prep into the ear canal. Okay, scrubbing solution? Yes.
CHAPTER 2
So, we're going to begin our stapes procedure with a 4-quadrant, or circumferential, canal block, which we begin right at the - just inside the meatus - just prior to where it transitions from hair-bearing to non-hair bearing skin. Occasionally, if the patients are a little bit more light, I'll warn them before injecting this as they may feel a little bit of the local anesthetic. And we're just going to march around the meatus. And as you're injecting, you want to see that, sort of, thicker meatal tissue expanding a little bit from the anesthetic. Okay, now the 5, Lorna. Next, I’m going to use a little bit smaller speculum to dilate the canal a little bit, but as I push in, it will milk this anesthetic down the canal wall. And you can now see some of this local anesthetic has kind of infiltrated down the vascular strip here towards the malleus handle. Okay. Back to a… There we go. Table towards me, please. This is a 6-mm speculum that we have in right now. Ideally, if you can get at least a 6, or even larger, that's a good working space. We’re using a transcanal. Other approaches that can be used are - endaural approach or a postauricular approach. I prefer to do stapes surgery through a transcanal approach using an ear speculum. Okay, injection now. Next, I’m going to inject a little bit more along the vascular strip, so - in the posterior-superior quadrant of the ear canal, just at about the level of the bony cartilaginous junction, I'm going to go in until I feel the needle hit bone. And then very slowly I will infiltrate, and if you can see down, you'll now see blanching of the malleus handle. And the malleus all the way down to the umbo will slowly blanch. And now we have a nice injection of our vascular strip.
CHAPTER 3
And to begin the surgery, we’ll make our canal incisions for our tympanomeatal flap - a 1 knife, please. We’ll make an inferior incision at approximately the 6 o’clock location, or as far anterior as we can. This is down to the level of the tympanic membrane. I'm going to make this incision just lateral to the annulus and then come straight out in the canal. And we’ll make three passes along this incision line right down on bone. Now a large round knife. And with our round knife, we will now make our tympanomeatal flap incision. As this cut is being made, we're kind of making small cuts and then lifting up and then connecting those cuts. So almost like perforating the skin successively and then connecting the - suction - connecting the cuts. Suction back. Suction, Lorna. And we’re going to continue all the way around, and I'm - as I'm making these cuts, I'm going right down to bone. Then I'm going to gently start elevating here. We're going to curve this cup - cut up superiorly. Oftentimes, you can cut this with a pair of scissors where it gets thicker up top. Suction now. Okay. Next, I’m going to start elevating the tympanomeatal flap. And as I elevate, I'm keeping this round knife right down on bone and pushing forward. And I'm going to actually get under the thicker part of the flap up top here and elevate. It’s a little bit swollen with our local anesthetic. And we’re just pushing forward. Bellucci’s to the right. Occasionally, the tissue more superiorly is a little bit thicker, and it’s helpful to trim some of this with a pair of scissors. There we go. And we're going to now elevate the flap inferiorly. And as I'm elevating, I'm going to suction on the back side of my round knife. You would like to avoid suctioning on the flap as much as possible to prevent it from getting more swollen or from possibly perforating it if it's very thin skin. And so I'm elevating now all the way down to the level of the annulus. I'm looking for the annulus inferiorly. There’s our tympanomastoid suture line. I'm going to continue elevating this flap all the way down to the level of the annulus. And then I'm going to slowly start pushing up with this round knife to try to get this underneath the edge of the annulus. There we go. I can see the annular ligament right there. There's a little bony ledge still there. Here I've got - there’s the edge of the annulus, here. And now I'm going to slip this underneath the annulus, and then I'm going to lift forward and up. And now I am under the annulus, and I'm going to keep elevating the annulus inferiorly to about the 6 o’clock, 7 o’clock location. That will allow us to really get our tympanomeatal flap up and over. Now a small BB-like cottonoid. At this point, I'm going to take a small cotton ball soaked in epinephrine and place this inferiorly. Gimmick now. This - often, you'll have bleeding from the inferior aspect where you've elevated your annulus. So this serves as a way of just tamponading some of that bleeding, and the epinephrine helps control that as well. There is like some skin on there. And we’ll just sort of press that into that inferior sulcus. Okay, now - we’re going to look back up superiorly and elevate the remaining portion of our tympanomeatal flap. Can I have a round knife, please? Okay, now a small Crabtree dissector. There is our chorda tympani nerve. And I’m going to carefully separate this fibrous tissue from the chorda tympani. And the posterior malleolar ligament. A 1 knife, please. There is the chorda tympani and a little remnant of the posterior malleolar fold. Let’s have a footplate hook now. We can start to see our incus and capitulum of the stapes. I’m going to just come through this little fold here, and also free up this chorda a little bit. There is the chorda tympani. The chorda tympani nerve. Okay, now a House curette.
CHAPTER 4
So next, to improve our exposure, I’m going to - we're going to remove some bone from the posterior-superior canal wall. Ideally, you'd like to be able to see the facial nerve above the oval window and the pyramidal process of the stapedial tendon posteriorly. Wipe. And this is a - as you curette, we’re - it's a rotational movement of the wrist. Just sort of scoop that bone out. Suction. And now a - a gimmick. I’m going to gently push this flap forward a little bit more - to give us some more exposure. And if we gently lift up on the malleus, I have good movement of the incus, but the stapes does not seem to move. The stapes is fixed. Suction. And I'm looking now for a round window reflex, but I really am not seeing much of one. Okay, so the stapes is fixed. We can go ahead and open the laser fiber. Curette. Suction. I can’t quite see. You see the anterior arch - very prominently. Oftentimes, you - you will not see the anterior arch that well. Yeah, I’m just curetting a little bit of additional bone to really try to be able to see the - more of the posterior aspect of the stapes. Yeah, because, see? He’s got a weird looking stapes, actually. And a very thin incus. Yeah. Very flimsy.
Okay. So now that we have improved exposure, I can see we have incus here. The incudostapedial joint - when you gently touch, you can see the joint stretch right here. The stapedial tendon, the anterior crus, and the posterior crus back here. The facial nerve can be seen medial to the incus here. Laser.
CHAPTER 5
Next, we’re going to separate the incudostapedial joint. This is a CO2 laser carried through a fiber optic - cable. And we are using settings of 4 watts and 100 milliseconds - pulses. Laser on. Laser on. I like to use laser to first sort of vaporize the mucosa surrounding the joint. Sometimes, it can be quite thick, and when you're trying to cut through it with a knife, you can be pulling on the stapes quite a bit. So I’m firing right at the level of the capitulum between the incus and the capitulum of the stapes. Incudostapedial joint knife now. Next, we’ll use an IS joint knife to - further separate the incudostapedial joint. If I lift up now, I get a nice, clean plane between the two. Good. Again, we have good movement of the incus and malleus. Laser back. Next, we’ll cut the stapedial tendon.
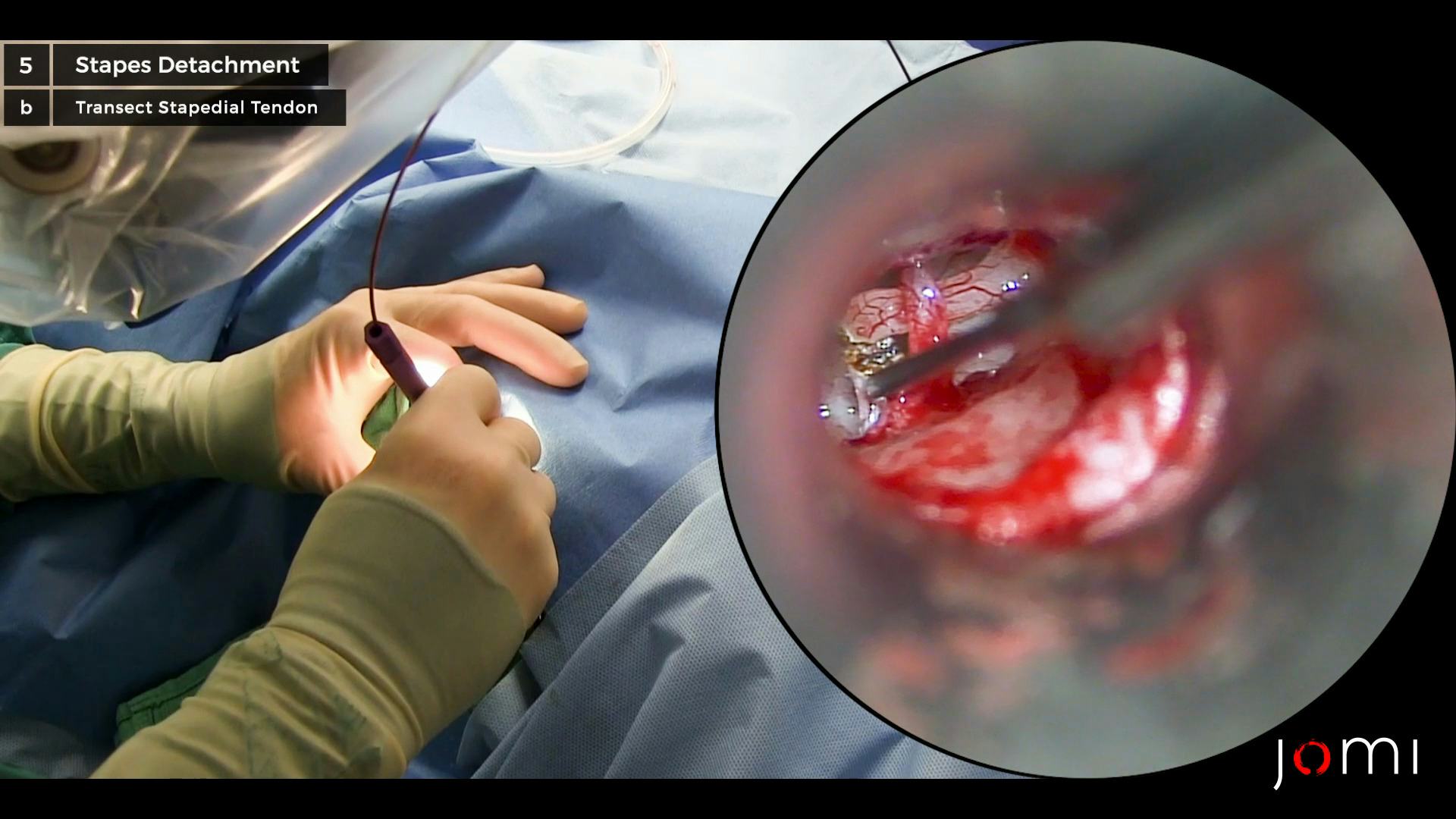
Laser on. Suction in my left hand. Very thick stapedial tendon. Once the tendon is cut, I can now have a nice direct line of sight at the posterior crus.
I’m going to now use the laser to cut the crus as close to the footplate as I can. And Lorna, we’ll go to a 24 suction now. Mm hmm. Okay. Laser back. Laser on. So we still have a few more areas of this posterior crus we’re going to laser now. And then this is an unusual - somewhat unusual situation where we actually have a very clear view of the anterior arch. Often just due to the angle, you can't see the anterior arch as well. Laser. So this affords us the opportunity to actually go ahead and cut the anterior arch with the laser as opposed to actually fracturing it. Laser on. So now I'm going to use the laser to go through the anterior arch. Again, we want to try to cut through as close to the footplate as possible, so we're not leaving too much of a remnant of the crura still attached. Now a Barbara needle. So next I'll use an instrument just to kind of break up these - this char that's still attaching the stapes. And now the anterior arch is separated, and next we’ll separate the posterior crus. And actually remove the - there’s still a little bit there. Laser. Okay, now the - crura is completely separated. Can I have a suction now? And we will just remove the arch of the stapes here. A pair of cups. I don’t think there’s enough suction on here. Okay, now a micro footplate hook. There is a little remnant of the - crura, so with a small hook we can kind of free that and clean that up a little bit. What’s that? Okay. And then we’re going to need a measuring rod next. Yep. Man, he is moving. Okay. Next, we’re going to measure the distance from the incus to the footplate. This is a 4.5-mm measuring rod, so it's 4.5 mm from the tip of this instrument to the small barb. So when measuring, this small barb should reach the top of the incus. And it may be a little bit - just a hair short. It's just about right actually. It’s probably going to need about a - do we have a 4.75 by 0.5?
CHAPTER 6
Next, we’ll use the laser to make our fenestra. We're going to make the fenestra in a - approximately the mid-portion of the footplate. He does have a lot of little blood vessels here, so we’ll actually use the laser to coagulate these. Laser on. And then... His footplate is actually pretty thick. Let's have the prosthesis next. And a little bit of water. Okay, now the posigator. Okay Lorna, hold that. And then a Barbara needle next. Thick stuff still. I’m actually scraping some of the char off of where we’ve lasered. This back part is thicker than it is anteriorly. Now a 24 suction, and then I'll take the laser back. And when I'm suctioning, I have my hand off of the control hole, so we have low suction. Okay, laser back. Laser on. Yeah, that’s very thick. I don’t know how easy that’s going to come out. See how it’s a little bit mobile with the… Yeah. Try to break up and get that char off of there. Suction now. Nah, that’s a footplate, but that’s okay. That’s okay. It’s a weird footplate. Suction now and then the laser. It's a lot thicker than it looked. Okay, now I'm starting to get through. We use it to actually make the opening bigger. Wipe, Lorna. He’s got a pretty big - yeah, I mean, a very thick footplate. So with this rasp, I'm going around the margins of our fenestra and just sort of smoothing out these edges. As much as I can. Fortunately, we have not had any bleeding. That's quite a... We have our fenestra now. Can I have the 6 mm now? Our piston we’re going to be using is a 5-mm piston, so we want to make sure it's going to fit in there. This is a 6-mm rasp. Wipe. I’m just about able to get that through there. Okay. The footplate is trying to come out. And next, we’ll take the prosthesis.
CHAPTER 7
Now can I have a footplate hook? So now, the piston is through our fenestra, and now we're just going to reposition the wire loop kind of where we want it on the incus. Maybe scoot it up just a little bit because it's... Usually, you want it at about the distal one-third, but his incus tapers a little bit towards the tip, and so you want to give yourself some distance so it doesn't have a tendency to slide off the bottom. And then I'm going to also just gently, before we crimp, make sure that it moves, and it does move freely within our fenestra. Okay, laser. This is a nitinol memory shape piston, so it is a wire loop that has a combination of titanium and nickel and when heated, will reassume a preformed shape. So we use the laser to actually crimp the prosthesis. Laser on. And we’ll just touch it a couple times. And then that should do it. Barbara needle. And we’ll just check and make sure that it's pretty secure on there. And there’s good movement of it with movement of the incus. Yeah, so the problem with most stapes prostheses - wire-loop type prostheses - is that if they’re crimped too tight, they'll strangulate the incus, and you'll get necrosis of the tip of the incus - or if they're too loose, the vibratory motion will gradually saw through the incus, and they will then fail. Bucket handle prostheses avoid this problem just by their - the inherent way that they sit onto the incus, so that is a different alternative. Although, they can have issues as well with other problems. Unfortunately, no one has developed a 100% foolproof stapes prosthesis.
CHAPTER 8
Next, we're going to take a little bit of subcutaneous tissue from the thicker area underneath our tympanomeatal flap, and just put a little bit of tissue around the base of this prosthesis, and then we will be done. Can I have a pair of cups to the right and Bellucci's? Yeah, can we wake him up a little bit, guys? That’ll be kind of cool. Okay, cups to the right. Bellucci's to the left. So I usually will go just to this thicker area of the tympanomeatal flap, vascular strip area. You can also take subcutaneous tissue from just inside the meatus, make a small incision, or you can take some subcutaneous fat from the earlobe. So just a small amount of tissue from here. Gimmick, please. Fascia press. Gimmick first. Bulb irrigator, Lorna. And then we’re going to press this small amount of tissue out. You don't have to do this necessarily, but I like to divide it into a couple small pieces. 59 - 10. Okay, now a Barbara needle. Here’s your knife, Lorna. And let me just leave that down for one second. And I'm just going to place a little bit of this subcutaneous tissue around the base of the prosthesis just to help form a seal. And that other piece. We’ll probably move back around to the front side. Okay. Suction one more time. Is that - 24? And then finally - the last thing we will do - Lorna, let me have that Barbara one more time - is we’ll just induce a little bit of bleeding to also form a blood patch around this prosthesis. I just want to check one thing. Hold that, Lorna. So the final thing we're going to do is just anterior to the oval window - find a little blood vessel and just avulse that a little bit to induce some bleeding, and then we'll form a little blood patch around this prosthesis as well. I'll just get that blood to come down. All right, Lorna, let me have a 3 suction now. So we have now soft tissue around the prosthesis as well as a blood patch. And we’re going to get our cotton ball out, and then we’ll be all done. Lorna, can I have a - can I have a pair of cups? Take that. Lorna, do you have another 3? Okay. Next, table away - and the ointment now. And then for filling the ear canal, we use Bacitracin ointment loaded into a 3-ml syringe with a blunt tip needle, and basically fill the whole ear canal with this ointment, and the weight of the ointment will just hold that flap down and allow things for healing.