Parotid Dissection (Cadaver)
,
Duke University Medical Center
Main Text
Table of Contents
Salivary gland tumors are uncommon, representing less than 4% of head and neck tumors. However, over 80% of these tumors arise from the parotid gland making parotid dissection an important tool for training surgeons to practice. Due to the rarity of these tumors and need for long-term follow up, specialized centers treat many of these patients. It is vital for surgeons to have a simplified, adaptable approach to parotid dissection. Additionally, a standardized approach to parotid dissection enables surgeons to adapt to different mass characteristics, which may become apparent during a case. In the video, we present a standard approach to parotid dissection using a cadaver. The patient described in the manuscript is a hypothetical case, and the information does not belong to the cadaver.
parotid neoplasms; facial nerve; otolaryngology
Tumors of the salivary glands comprise less than 4% of head and neck tumors.1 Most salivary gland tumors occur in the parotid gland with over 80% being benign.1,2 For benign parotid tumors, superficial parotidectomy is the standard approach to resection depending on their location within the gland. Surgical planning aides such as fine-needle aspiration (FNA) and imaging cannot always provide a definitive diagnosis for the malignant potential of a mass but remain a vital step in the workup of these masses. For this reason, surgeons should be prepared to convert to a total parotidectomy.3 Even for benign lesions, total resection of the mass is imperative as certain pathologies, such as benign mixed tissue tumors, can recur.4 A standardized approach to parotidectomy that preserves the opportunity to convert the procedure is an important skill for head and neck surgeons to develop.
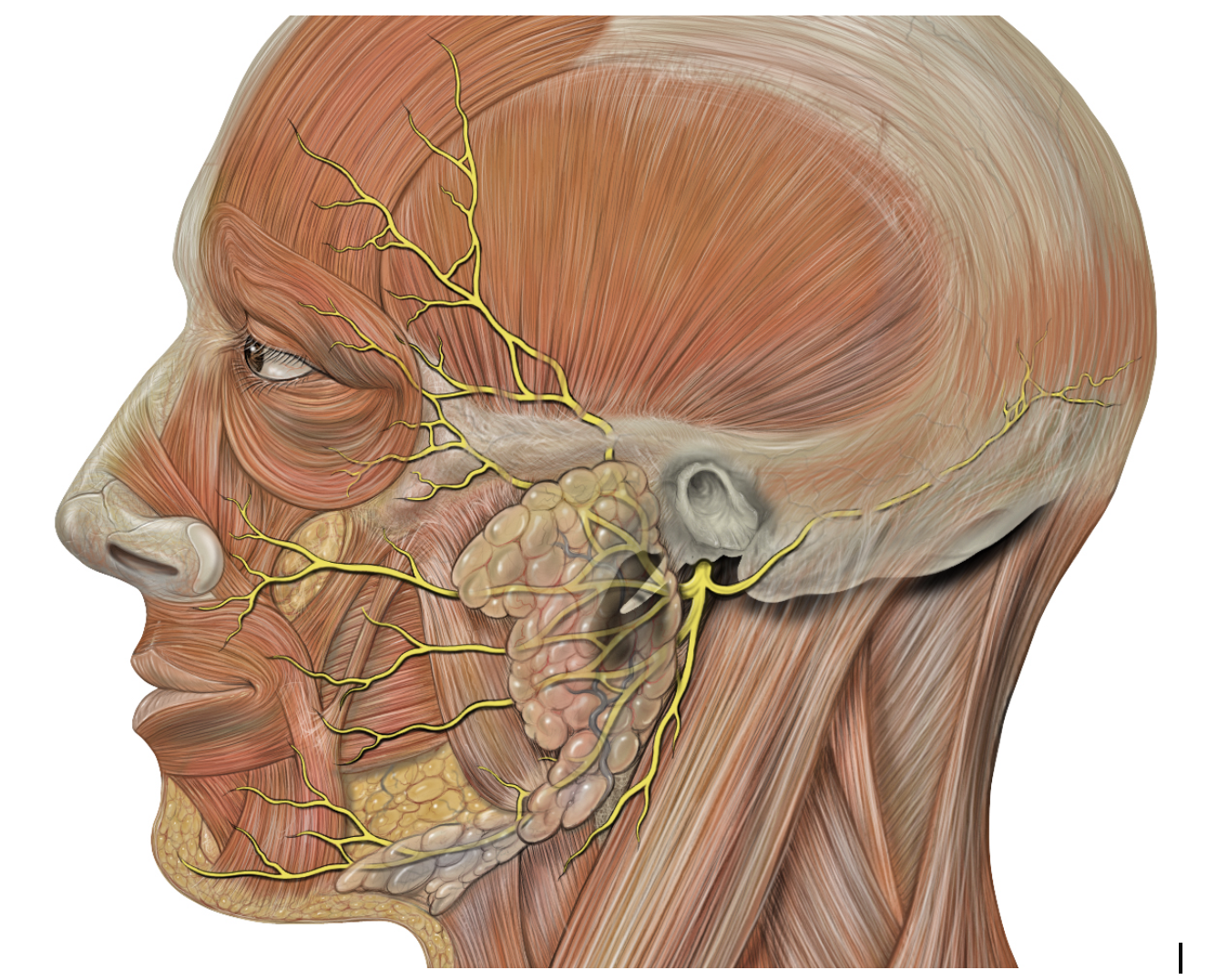
Figure 1. Anatomy of the Facial Nerve in relation to Parotid Gland.Patrick J. Lynch, medical illustrator, CC BY 2.5 <https://creativecommons.org/licenses/by/2.5>, via Wikimedia Commons
A standardized approach to parotidectomy is particularly important to minimize risk to structures in the surgical field. The facial nerve is the primary critical structure enmeshed in the parotid gland. It serves as a critical landmark that artificially divides the superficial from the deep lobe of the parotid.2 Nerve stimulatory control units and nerve integrity monitoring systems provide intraoperative stimulation and monitoring. These tools assist with the identification of the facial nerve and confirmation of its integrity but should not replace a surgeon’s anatomic knowledge of surrounding landmarks. For this reason, the surgeon must confer with the anesthesiologist to ensure long-acting paralytic agents are not used. Methods and landmarks to identify the facial nerve intraoperatively include the tragal pointer, the tympanomastoid suture line, retrograde dissection, the tragal ‘pointer,’ and the digastric muscle.
A 39-year-old female presents with a mass on the left lateral side of her face that has grown noticeably over the past 2 years. The patient believed it was a small sebaceous cyst. However, as the mass continued to grow, she sought care from her family physician. She reported no other symptoms. She does not smoke. She does not have a history of cancer or radiation to her head and neck. Besides the mass, her history is unremarkable, and she does not take any daily medications. Her family physician referred her to otolaryngology due to the concerning location of the mass.
On exam, the patient had a 3.6x3-cm mass on her left lateral face. The mass is fixed and non-tender with no erythema. Cranial nerves II–XII are intact. She has no cervical lymphadenopathy. Aside from her primary lesion, the rest of her face and skull is symmetric.
An ultrasound of the lesion demonstrated a hypoechoic mass and a fine needle aspiration was consistent with pleomorphic adenoma but was not definitive. Therefore, additional imaging was recommended. I have never seen a case of FNA deferment due to concern of facial nerve damage.
A computed tomography scan demonstrated a homogeneously enhancing lesion measuring 3x2.5-cm overlying the left parotid gland. On magnetic resonance imaging, the mass appeared heterogenous on T1 series with hyperintensity on T2 series. The combination of imaging and pathologic findings was consistent with pleomorphic adenoma.
Pleomorphic adenomas, also known as benign mixed tumors, represent 84% of benign parotid masses.5 Approximately 75% of pleomorphic adenomas originate superficial to the facial nerve.6 Superficial tumors can progress to the level of the deep parotid lobe generating a dumbbell-shaped mass on imaging.
Pleomorphic adenomas originating from the deep lobe have unique characteristics compared to their superficial counterparts.7 (What are these unique characteristics? Why would this statement be added with a reference without including the specifics of the comment).
The treatment for pleomorphic adenomas is surgical resection with parotidectomy. It is important to maintain a clear margin of tissue without violating the capsule of the tumor to avoid recurrence or potential “seeding” of the mass with multiple areas of recurrence. A partial superficial parotidectomy may accomplish this goal depending on the size of the mass.3 If a tumor cannot be definitively excised from surrounding tissue, the surgeon should be prepared to convert to a total parotidectomy. Regardless of approach, the facial nerve should be carefully dissected and preserved unless tumor characteristics necessitate sacrifice of the nerve.
Postoperative radiation therapy has been explored for pleomorphic adenomas. Most examples of this practice involve patients with margin-positive resections, recurrent pleomorphic adenomas, or challenging tumors that are enmeshed with the facial nerve.8–10 The decision to pursue this treatment should be determined upon consultation with the patient, a radiation oncologist, and a head and neck surgeon to assess utility and necessity.
Recurrence rates of pleomorphic adenomas after parotidectomy range from 1–4% for superficial parotidectomy and below 1% for total parotidectomies. 11,12 Most recurrences occur within 18 months of resection. Therefore, appropriate and consistent follow-up particularly within the first 2 years post-resection is advised. Recurrent pleomorphic adenomas often appear as multiple small tumors found along the path of surgical excision and can be mistaken for adenopathy initially. The mechanism of the apparent tumor seeding is still under investigation with the working hypothesis being that residual tumor cells may be left behind and regrow or secondary to capsule violation. Interestingly, pleomorphic adenomas that originate from the deep lobe appear to not have as high as a risk for recurrence even when only enucleation is performed.7 It is vital that treatment for this tumor type removes all pathologic tissue with a perimeter of normal tissue to minimize recurrence.
Contraindications to parotidectomy alone include distant metastatic disease and tumor invasion of the parapharyngeal space, mandible, skin, or ear canal. These other situations may necessitate a combined approach with other surgical specialties. Metastatic pleomorphic adenoma, while rare, may be responsive to radiotherapy after resection of the primary tumor.10
Large pleomorphic adenomas that invade other compartments will require more extensive surgery than a standard parotidectomy.
With the starting incision, cosmesis and exposure are important to consider. By utilizing a “Gull-Wing” incision to mitigate tissue contraction and by hiding the incision in the hairline and skin creases, surgical scars can become imperceptible. However, the initial incision may have to be moved to a more visible area depending on the location of the mass.
As the tissue flap is raised at a level dependent on the level of the mass, important landmarks include the external jugular vein and great auricular nerve. Identification of these landmarks allows for preservation of the nerve as long as no tumor encroaches upon it. This can achieve preservation of sensation to the inferior aspect of the ear. With the nerve identified, the parotid fascia can be dissected from the perichondrium of the external auditory cartilaginous canal. This allows continued exposure of the tragal pointer, which is vital for identification of the facial nerve as the nerve courses 1 cm anterior and inferior to the tragal pointer in normal anatomy.
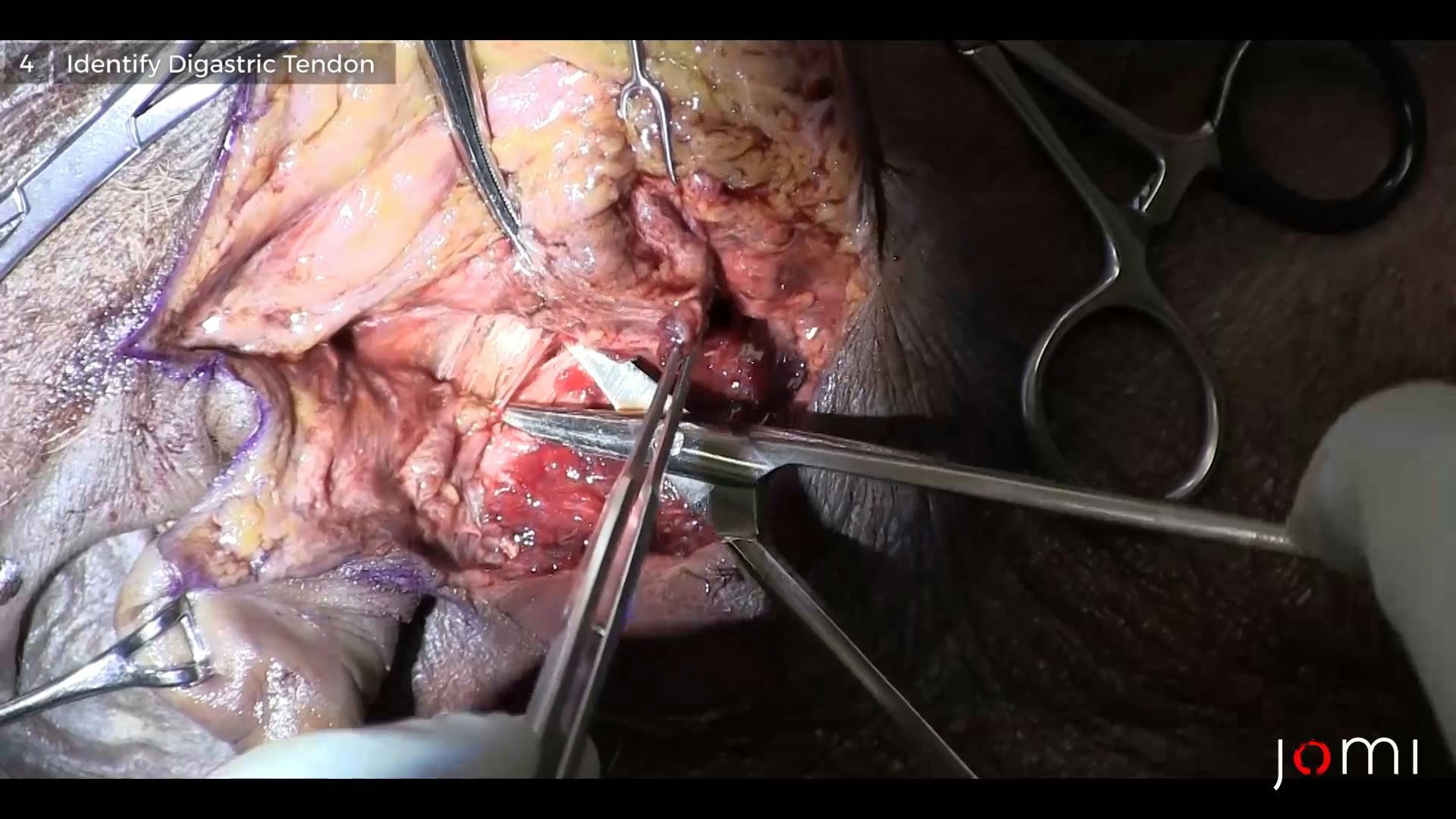
The digastric muscle is the next important landmark, which helps identify the common facial vein anteriorly and also demarcates the level of the facial nerve in the parotid. Finally, the tympanomastoid suture can be palpated, which if followed to the styloid process would transect the facial nerve. The authors prefer to identify this structure but not use it as a dissection plane due to its depth. Instead, after identifying the three key structures, the parotid fascia can be cut superficially and bluntly dissected from the posterior belly of the digastric muscle to the anticipated location of the facial nerve. Care should be taken to avoid the transverse facial artery which exists in the same plane. Once the facial nerve is identified at its main trunk, the upper division of the facial nerve can be dissected (the primary branch point of the facial nerve into superior and inferior divisions is referred to as the ‘pes anserinus’). This is challenging due to the superficial temporal vessels, so it is advised to dissect along the superior portion of the facial nerve rather than on its lateral surface. Attention is then turned to the lower division. Identification of the retromandibular vein and posterior facial vein can aid in identifying the expected course of the marginal mandibular branch as this nerve lies superficial to the veins.
After completing superficial dissection, the deep lobe can be dissected. The facial nerve should be mobilized off all the soft tissue in this region. Superficial temporal vessels should be controlled at this point. The deep compartment can be identified by locating the terminal branch of the external carotid artery and the posterior facial and retromandibular veins. The space deep to the facial nerve in this region is safe from damaging the facial nerve and allows for access to deep lobe tumors. The deep parotid can be separated from the posterior border of the mandible down to the styloid process. Deep vessels to control here include the internal maxillary artery and vein allowing the surgeon to free the deep lobe from the styloid process and parapharyngeal fat thus completing the dissection.
The presented dissection and accompanying case highlight important principles in parotidectomy. The standard approach presents possible variations in dissection based on tumor location. It allows for the conversion of the procedure to total parotidectomy. Finally, it provides systematic assistance to identify important landmarks and safely locate the facial nerve.
Regarding the case, treatment for pleomorphic adenomas has improved as evidenced by the decrease in recurrence. As mentioned, current rates of recurrence are consistently less than 4%; however, historically the recurrence rate was 20–45% when only enucleation was performed.6,11 The adoption of parotidectomies is credited for this accomplishment.
Superficial parotidectomy lasts approximately 2 hours. Minimal blood loss is anticipated during the procedure ranging from 40–60 cc. The head of the bed can be elevated to minimize bleeding.13 The modified Blair incision is most used. For ideal cosmesis, the incision should follow the natural creases of the neck depending on the need for neck dissection or be placed along the hairline particularly in individuals with long hair.14
Closure of the wound should include placement of a surgical drain. Drains can be removed when output is 10 ml or less per day. These drains can be removed on an outpatient basis if the drain output goal is not reached during hospitalization. In relatively small parotid tumors, these drains are often removed in the morning or afternoon on the day after surgery (postoperative day 1).
Important complications include facial nerve paralysis and/or permanent facial nerve damage. If intraoperatively the nerve is confirmed intact, but the patient still experiences weak neuromuscular responses to stimulation, it is likely they will make a full recovery.2 Mild neuropraxia should resolve in 4–6 weeks but may require longer depending on traction placed on the nerve during surgery. Consultation with physical therapy for facial nerve rehabilitation may be beneficial in such patients.
Other possible complications include Frey syndrome, salivary fistula, facial asymmetry, first bite syndrome, and other standard surgical risks such as bleeding, infection, and complications of anesthesia.
Most patients can be discharged within 24–72 hours after the procedure. Patients return to the clinic in 1 week to discuss results from pathology, establish follow-up timeline, and have sutures removed if non dissolvable sutures were used. Additionally, patients are advised to avoid acidic foods for 6–8 weeks after surgery to allow the parotid gland to recover.3 There is no clear consensus on when to perform surveillance imaging for recurrence. Often, biannual physical exams alone are sufficient to detect new masses suggestive of recurrence. Long-term relationships develop between surgeons and their patients as recurrence can occur 10 years or more after resection.
Standard special equipment utilized for this surgery13:
Jackson-Pratt bulb suction drain or TLS drain
Shaw scalpel
Nerve stimulator control unit and instrument (Parsons McCabe)
Nerve integrity monitoring system (NIMS)
C. Scott Brown also works as the lead editor of the Otolaryngology section of the Journal of Medical Insight.
This case is a standard parotid dissection demonstrated on a cadaver; no consent was required. All other persons seen in the video consented to publication of the media.
Citations
- Jennifer R. Wang, Diana M. Bell, Ehab Y. Hanna. Chapter 84: Benign Neoplasms of the Salivary Glands. In: Flint PW, Haughey BH, Lund VJ, et al., eds. Cummings Otolaryngology-Head and Neck Surgery. 7th ed. Elsevier; 2020:1171-1188.
- Galati L. Chapter 92: Superficial Parotidectomy. In: Myers EN, Snyderman CH, eds. Operative Otolaryngology-Head and Neck Surgery. Third edition. Elsevier; 2018:613-617.
- Ashok R. Shaha. Chapter 3: Superficial Parotidectomy. In: Khatri VP, ed. Atlas of Advanced Operative Surgery. ; 2013:23-28.
- Patey DH, Thackray AC. The treatment of parotid tumours in the light of a pathological study of parotidectomy material. Br J Surg. 1958;45(193):477-487. doi:10.1002/bjs.18004519314
- Spiro RH. Salivary neoplasms: overview of a 35-year experience with 2,807 patients. Head Neck Surg. 1986;8(3):177-184. doi:10.1002/hed.2890080309
- Rosai J, Ackerman LV. Chapter 12: Salivary Gland. In: Rosai and Ackerman’s Surgical Pathology. 10. ed. Expert consult. Elsevier, Mosby; 2011.
- Harney MS, Murphy C, Hone S, Toner M, Timon CV. A histological comparison of deep and superficial lobe pleomorphic adenomas of the parotid gland. Head Neck. 2003;25(8):649-653. doi:10.1002/hed.10281
- Chen AM, Garcia J, Bucci MK, Quivey JM, Eisele DW. Recurrent pleomorphic adenoma of the parotid gland: Long-term outcome of patients treated with radiation therapy. International Journal of Radiation Oncology*Biology*Physics. 2006;66(4):1031-1035. doi:10.1016/j.ijrobp.2006.06.036
- Armitstead PR, Smiddy FG, Frank HG. Simple enucleation and radiotherapy in the treatment of the pleomorphic salivary adenoma of the parotid gland. Br J Surg. 1979;66(10):716-717. doi:10.1002/bjs.1800661012
- Patel S, Mourad WF, Wang C, et al. Postoperative radiation therapy for parotid pleomorphic adenoma with close or positive margins: treatment outcomes and toxicities. Anticancer Res. 2014;34(8):4247-4251. PMID: 25075054
- Laccourreye H, Laccourreye O, Cauchois R, Jouffre V, Ménard M, Brasnu D. Total conservative parotidectomy for primary benign pleomorphic adenoma of the parotid gland: a 25-year experience with 229 patients. Laryngoscope. 1994;104(12):1487-1494. doi:10.1288/00005537-199412000-00011
- Witt RL, Eisele DW, Morton RP, Nicolai P, Poorten VV, Zbären P. Etiology and management of recurrent parotid pleomorphic adenoma. Laryngoscope. 2015;125(4):888-893. doi:10.1002/lary.24964
- Parotidectomy with Facial Nerve Dissection. Iowa Head and Neck Protocols. Published April 29, 2020. Accessed January 27, 2021. https://medicine.uiowa.edu/iowaprotocols/parotidectomy-facial-nerve-dissection
- Zhang J, Jiang Q, Na S, Pan S, Cao Z, Qiu J. Minimal Scar Dissection for Partial Parotidectomy via a Modified Cosmetic Incision and an Advanced Wound Closure Method. Journal of Oral and Maxillofacial Surgery. 2019;77(6):1317.e1-1317.e9. doi:10.1016/j.joms.2019.02.036