Pediatric Bilateral Indirect Inguinal Herniotomy
Transcription
CHAPTER 1
We have a 12-year-old boy, with an indirect inguinal hernia, which presented at birth, meaning to say that this child has a bulging mass at the left inguinal area since birth. He was seen by a physician and it was a clinical diagnosis of inguinal hernia. Inguinal hernia is the most common pediatric surgical conditions, not only in the Philippines, but also in other parts of the world, in the US and other countries. And most common procedures that we are doing is repair of the inguinal hernia or we term as herniotomy or high ligation of the sac. So, now we have marked the type of incision- and by the way, this boy has a bilateral hernia. So, we'll do the operation on both sides, me first and next is by Dr. Rahdu, okay?
CHAPTER 2
We'll start now, after marking the incision, this will be in the crease line, on or above the suprapubic area. So, these are the markers, the suprapubic area and the midline. And we do an incision from this side for the left, inguinal hernia. So, we'll start the incision. Cutting. So we are now cutting the skin.
CHAPTER 3
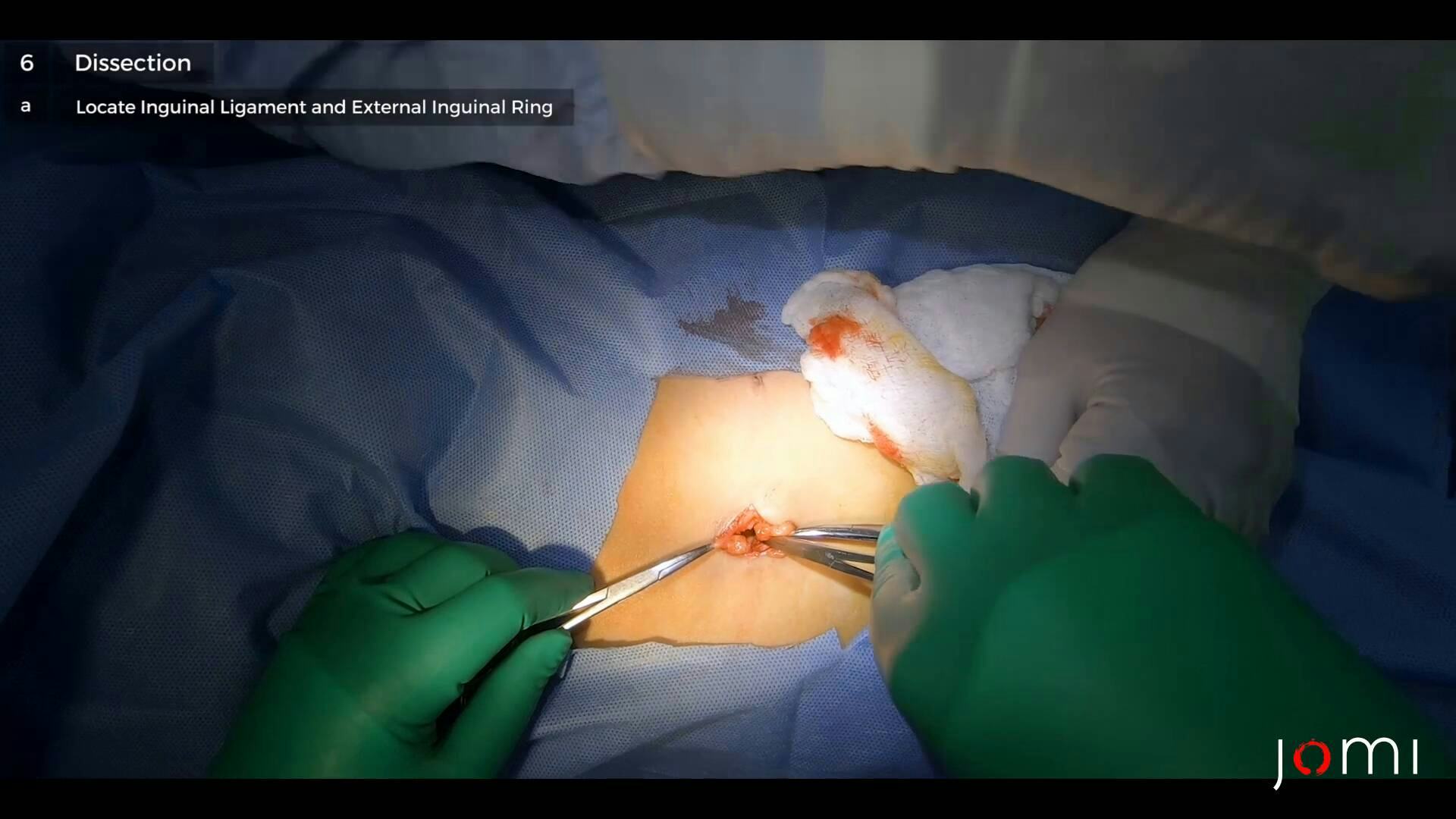
So the- we expose the subcutaneous tissue. The subcutaneous tissue is composed of the following layers: This is the Camper's and we are now exposing the Scarpa's fascia. So we do the incision and opening layer by layer. So we expose now the external oblique, So we are now at the level of the external oblique, we're looking for the inguinal ligament, that's the landmark. So, if you can- the shelving edge of the inguinal ligament, we're trying to expose this one and that will be the marker where- to look for the external ring. So this is now the part where we will open and to look for the external…
So, we have put the clamp on the opening of the external inguinal her- ring- the external inguinal ring. We're trying to open it. Mosquito clamp.
So we have opened the external ring, and now we're- and now we're looking for the… We're looking now for this spermatic cord. This is a very important landmark in the inguinal dissection, where you have to look for the spermatic cord. Spermatic cord is where the hernial sac, spermatic vessels, and the vas deferens is the composition of the… So, I have- put my clamp on the spermatic cord. I'm trying to separate each component. As I mentioned, the components are the hernial sac, and the spermatic- spermatic vessels, and the vas deferens. No. The hernial sac- the origin of this is the processus vaginalis, which came from the peritoneum or the peritoneum as the testis goes down embryologically, it carries with it part of the peritoneum. So, the peritoneum that goes down with the- with the testis is called the tunica vaginalis. We're pushing away the cremaster muscle. Yes, we're separating the spermatic cord, which is now covered, or you'd say it's enveloped, by the- sperm- cremasteric muscles. That's what we're doing now, so that we can totally isolate the spermatic cord. Maybe I was pulling the wrong testis, this one. Yes, this one. Yes. So you can see here in the camera that we have exposed now the spermatic cord, which is composed, as I mentioned, the spermatic vessels, that's what I'm holding now.
And now I'm trying to look for the hernial sac, which usually is located on anteromedial, this is the medial portion. And we're trying to separate it from the vessels. Why? Because we have to ligate the hernial sac, as I mentioned. The high ligation is the correction of inguinal hernia in children, which is very different from the adults. So, anatomically you can identify the vas deferens, this is the vas deferens. This is the spermatic- pampiniform plexus. Those spermatic vessels, and now we're looking for the hernial sac. The sac is the one to be ligated. Should we separate them? It's not under. We didn't go through it, but isolate… So, this is the- so identifying again, the structures of the spermatic cord, we have put the clamp on the hernial sac. This is the structure we have to ligate. And next is the vas deferens. Yes. Which they couldn't do it where the sperm goes to the testicles, and this is the vessels, pampiniform plexus, so we'll separate it from the hernial sac. Okay, so, now we… Now, dissect the hernial sac down more approximately up to the level of the internal ring. We have to do the ligation as high as possible, and the landmark for this, the- peritoneal line. Or as the peritoneum exits the internal ring. So we have now, cut the part of the sac, and we're- I'm trying to- to do a farther dissection- farther dissection so I can identify the preperitoneal fat or- the, what we call the white line of Toldt. So, this is still- so this is the part where it goes down to the peritoneal cavity.
So, that will end our dissection, and I will now ligate this structure. We used Vicryl. It's an absorbable suture. So I place my suture on the most proximal part of the hernial sac. So, it's called high ligation. So we call it high ligation of the sac, the proper terminology for the correction of inguinal hernia in children. It's an indirect inguinal hernia, which is different from the adult inguinal hernia, which are usually a direct type of hernia. A direct type of hernia, secondary to weakness of the muscles. So this is the cystal side, so we just leave it. So we have finished now the ligation, and practically that ends the hernia repair, now we, we'll now close the layer- each that we have incised, okay?
CHAPTER 4
So, again, identifying the external oblique muscles, and now- close it by layers. So we just approximate the layers of the external… Spermatic vessels. We're closing now the subcutaneous tissue. So we're doing a subcuticular continuous suture on this side. So, we're almost done with the repair of the hernia on the left side. Almost done, and- we're now going to the other side, the right side.
CHAPTER 5
So we're going to start now with the operation on the right side, So I make an incision through the skin. A bigger incision because it's a bigger hernia.
CHAPTER 6
So, this is your Camper's fascia, it's actually- part of your sub-q. So, we look for the Scarpa's fascia, which is actually still part of your subcutaneous tissue, but it can sometimes fool us into thinking that it's- because it's thick in children, so we mistake it for the external oblique aponeurosis. Retractor, yes retractor. Retractor. Other retractor, please. So that's your external oblique aponeurosis. So, we dissect, we clean out the external oblique. And we go lateral to look for your inguinal ligament. So it's your external oblique aponeurosis that curls in on itself. So your external oblique aponeurosis will curl in to form your inguinal ligament. So, that's what we call… That's what we call our shelving edge. And if you follow that down and medial, then you will see your external inguinal ring. This is the external ring. Knife please.
Clamp? In children, the aponeurosis is soft, so, it indents when you try to clamp. Metz, please. So we open it up, towards the ring.
So, open up the cremaster muscle and look for your spermatic cord. And so you slowly push away the spermatic - the cremaster muscle. So occasionally, when you have difficulty in identifying the spermatic cord, you have to... tug on the testicle and try to, and try to- push it up and down, like what I'm doing. So we can identify- the- spermatic cord. Spermatic goes down directly to the testes, to this scrotum, so when you hold the scrotum, goes scrotum, then you can more or less identify the spermatic cord. So, now she's holding the spermatic cord. I'm trying to separate the other layers again, layers as I mentioned, the hernial sac, the spermatic vessels, and the vas deferens. Another Debakey please? It looks very thin. And we'll just push the muscles away. Small retractor. There's nothing inside. Yes. Let me pull it out some more. See, I like transferring my pickup. This side, it's kind of big, and the cord, so, we tried to deliver the whole cord out of the wound, so that we don't touch the- clamp, please? We don't touch the floor and create a direct hernia, because the floor in children is still intact. So this is your cord, much bigger than the other side.
So, the whole cord is usually covered by your spermatic fascia. Everything in the hernial sac, the spermatic vessels, the vas deferens so, you try to split- open your spermatic fascia and separate your cord structures from the sac. So this is now your sac, and these are your vessels, your pampiniform plexus, your spermatic, your testicular artery, and your vas deferens, so we hold onto the sac until we peel out the chord structures, unless you slowly, unless you slowly separate, you usually encounter to the vas last. So this is your vas deferens here. And, trying not to pinch the vas so you don't injury it, There, that's your vas deferens. Clamp, please. So once you've separated the other chord structures, you isolate… Where's my vas deferens? So, you isolate the chord structures, so you do not ligate them- ligate the structures together with your- clamp, please. They're stuck, so… Excluding the cord structures. So we can open this up, just to check if there are no structures inside. Okay, so you make sure that your cord structures are not close. Opening up the sac. So this is your hernial sac, another clamp? So, this is your distal sac. It's almost closed. And this is your proximal. It goes down to the peritoneal carvity. Clamp, please. Okay, so making sure there are no cord structures, we separate the proximal sac from your distal sac. See that, clear? Clear, so, close it. Okay, so... Retractor. Retractor. We pull away… We free the sac until we see the preperitoneal fat. Here, preperitoneal fat. And that's... The end. That means you're at the level of your internal inguinal ring, which is the level for your high ligation. And you tie it up.
Okay, so that's... Okay. Metz? So, now we're going to what? So, we're just going to trim the sac, and just drop it in, and that's it. That's it. And for the distal, just check… There's some hydrocele. It's very small, I think it's almost- about to become non-communicating. Let's see if there's any fluid, and there's none. So we just leave the sac as it is. Check for bleeders. So, we have ligated the sac on the right side, so we're now trying to close the external oblique again.
CHAPTER 7
Another clamp. Layer by layer, we're closing. We're closing the external oblique aponeurosis. And then, I don't usually close the sub-q separately. In hernial repair in children, you don't use non-absorbable suture, you usually use absorbable sutures. Because it's difficult to remove sutures in children when they're awake. You have to do a subcuticular sutures. And it's an absorbable one. So these are bilateral incisions- the other incision is the bigger one, because it's the hernial side, it's a bigger sac, and a smaller sac.
CHAPTER 8
Inguinal hernia is the most common pediatric surgical conditions that we have, as i may- not only in the Philippines, but also all over. So, herniotomy or hernia repair in children, it's practically just high ligation, it's very different from hernial surgery in adults. So, the- usually, the- on adult side, is a direct type where the muscle overlying the hernia is usually weak. So, you have- in adults you, you have to repair the, the muscle. But in children, you don't touch that one, just ligate the sac, and that's it, that's finished it now. We don't use mesh, as you can see the hernia repair in adults, later on there will be hernia repair in adults, and if you see that they're using a mesh structure to overlay, this more or less strengthen the muscle layer, that is the weakness of the hernia in adults. So, practically it's very- not really simple, but a very short procedure of hernia repair in children. And- this also can be present in, in a- in female, or in girls. So maybe 1 out of 10 of hernias in children are usually female. And the cause of the majority of these are genetics, meaning there's- passes genes from generation, maybe from the father or grandfather to his children. So, if you asked the parents, maybe his father, or his mother, or one way or the other, the siblings also had inguinal hernia. And in some cases, you can see that the mother, the- maybe the father, and all the children have inguinal hernias, So, that's the genetic point of hernias in youth. In adults, the majority of these are acquired causes, meaning those related to work, like lifting heavy objects, those are very athletic, and those with other collagen diseases, so these are the main causes that we see in adults. As I mentioned, these are the 2, even in adults, I think the most common, surgical... or repair, or procedures that they do in practice, is also a hernia repair. In children, just the same is statistics, okay? Whether you're in the rural or in the- city level or in the university, the procedure is the same, the same. The only difference is- maybe it- is in adults, because some now are using a laparoscopic repair of hernia, that we never do in children. Okay? Laparoscopic procedures in hernia is now the trend of hernia repair in adults, but they never do laparoscopic hernia repair in children.