Posterior Sagittal Anorectoplasty (PSARP) for Imperforate Anus
Transcription
CHAPTER 1
This is a case of patient- a 9-month old patient with an imperforate anus. So our planned procedure is a posterior sagittal anorectoplasty. So right now we're looking at the patient in a prone position. So we're trying to assess for any sphincter function, so this is the muscle stimulator. I'll say 200. Test. Test. Test. So this is a 9-month old male, who was diagnosed with imperforate anus. And an emergency colostomy was done, I think this is a sigmoid colostomy. Vicente Sotto? Yes. Vicente Sotto Memorial Medical Center. So- this was identified as a high type of fistula, because of the- the markings that was shown in the radio- X-ray and the lateral view, where the distal air was appreciated above the coccyx. So, for this case, after the colostomy, for around 1 to 2 months, you can now proceed with the procedure; however, this patient came at 9-months old due to financial constraints probably, and the lack of the sources or funds for the procedure. Now, this case is a high type, so we're doing definitely procedure of a posterior sagittal anorectoplasty in which we create a new anus for the patient. So, this leads- this is the second procedure, and the last procedure would be the closure of the colostomy. But with the definitely But with the definite procedure, we hope that we could do a- a posterior approach by pulling the remnant rectum to the- in doing the new anus, okay? So, if you do not have any silk available, 6-0, we use this as a marker- we use a cautery or a stimulator to check the patency of the muscles for the new anus. So we check for the posterior border, and then that- what I usually do is just- you might use it with a cautery instead of a suture. So this is- my markers, and this is my center. Okay, so this is your border posteriorly and then anteriorly the- skin.
CHAPTER 2
Cutting up. So we're now incising the skin, with a posterior sagittal incision, carried to the subcutaneous tissue. For pediatric patients, we use a blade 15.
CHAPTER 3
There's muscle stimulation. OS please, OS to me, please. So upon incising the skin and subcutaneous tissue, you look for the parasagittal fibers- up to the- muscle complex and the level of the posterior rectal wall. So this is the muscle. Increase- go up to 10, please. So we're still dissecting the ischiorectal fat. Do you have any retractor? And this is the coccyx. The distal tail of the- the distal tail of the spine. Do you have any retractor, ma'am? We're now going to adjust the… Reapply. Retractor please? Another retractor please. Reapplying the- Weitlaner. So we go along with our dissection. So we use the coccyx bone as our landmark posteriorly, the radiographic- the distal area is where it's located. Mosquito please. Mixter to me please. I'll readjust the… Okay. Do you have the Mixter now? Mosquito. Retractor please. We think this is already the distal rectum. So we're just dissecting around the fats- areolar tissues. We're just releasing all the fats connected to the distal rectum, so that you could release it anteriorly. So, sometimes you have to manually feel the- the bowel, sometimes you miss it as a bladder. You will feel the catheter inside if it is in the ureter and goes to the bladder Basically we use a Foley catheter to guide- help us guide in determining the rectum. If it has a balloon inside, definitely this- it's a bladder. We do not feel any tubing inside because we inserted the French 8 catheter. Probably this is already the rectum. It's okay? Mixter, Mixter. The Mixter. Suture this one if you want. Yes. So that you could pull the posterior rectum, and then we can open it as our guide.
CHAPTER 4
So we'll be using a silk, 3-0, round needle to tag the posterior rectum in order to guide us- dissect also the anterior portion of the rectum. It will also lead us if there is a fistula- to the-- a fistula is a cavity that connects 2 hollow organs, structures, specifically with this wall, it's probably- clamp- it's probably a rectourethral fistula. It's common in- in males, and in contrast, female is the rectoves- vestibular fistula, is common among females. Clamp. Scissors.
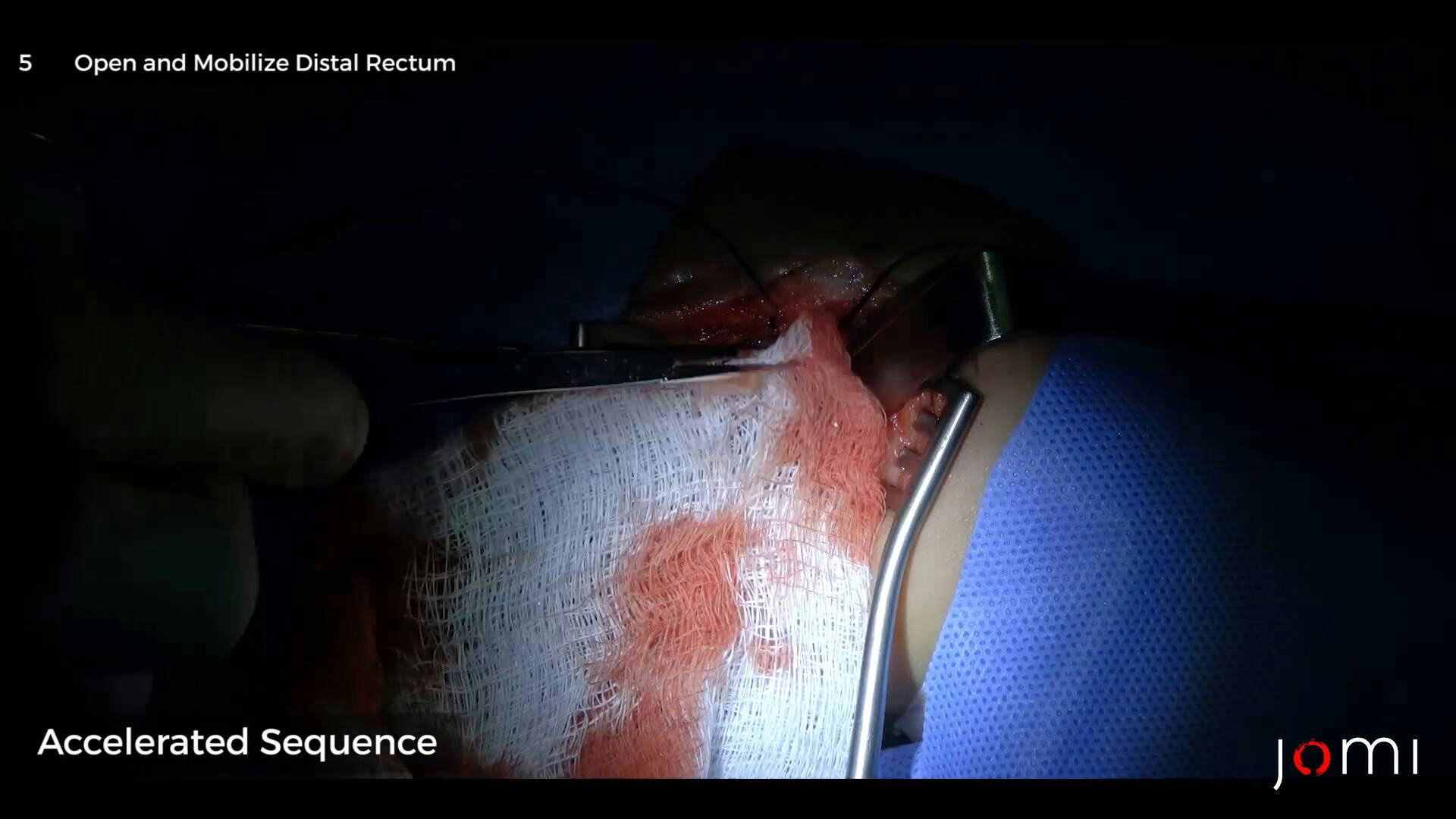
CHAPTER 5
We're now trying to open the distal rectum, if it is- it's the one structure that we'll try to- bring down to the skin, the muscles complex. Clamp. Yes, with the structure that we're see right now, I think... We can pull it down. We can pull it already, so- it won't open in the abdomen for the- for further dissection of the distal. I think we could bring this one here, and do the anoplasty later. Another suture. So we are just closing the... Initial opening that we made. Yes, the initial dissection for the rectum- because it's almost at the anterior portion of the- the bowel. Scissors. Dissecting again the posterior part of the rectum so we could lengthen the- the attachment to the anus. This is our soft tissues, we're trying to release it. We add another sutures for retraction anterior and posterior, and this are the lateral. So this is the anterior rectum ready, right? So, this is most likely the urinary complex, which is the bladder and the urethra beneath, you can feel the catheter inside, and this is the distal portion of the rectum. This is enough- distance… Retractor. To do the new anus already. Okay, this is the ischiorectal fat, this is the muscular complex.
CHAPTER 6
So we're just closing the ischiorectal fat anteriorly to close the- opening to the- peritoneum. So, I'm doing the- now that we have enough length of the rectum, we make sure that we have an- vascular supply of the rectum.
CHAPTER 7
And the same time it is... by placing these markers also for which- where we apply it properly, or it won't- if there's not enough tension, we do not reach the bowel. This time we are attaching the ischiorectal fat to the posterior rectum- for support. This is it- around 1 to 2 case in every 4 to 5,000 live births. Of course. We're almost closing the ischiorectal fat, and- and the last portion is the anoplasty.
CHAPTER 8
We're checking our markers posteriorly. And to lessen the technique in doing the anoplasty, we- we should anastomose the skin to the mucosa. This is our marker. Pickup. These are our markers. This is our border for the posterior anoplasty. We still have extra needle holders. So I'll be applying the cardinal sutures. So I'm closing the skin subcutaneously. Cut this. Opposite side. It's good, very good. Because this is mucosa- and the skin, and this is excess. Excess tissue. Cautery please. Half and then you can trim that one. If a patient is at 9 months old, you can have a dilator of a 13 and 14 dilator. So, we're looking for the size. Yes, 13 and 14. So, we apply first the 13. So this is a size 13 Hegar's. 12. That's a size 11. Now 12. 13. This is the right size for the patient. We're now cutting the- The cardinal borders. Can we check first the pena dilator, and then we will apply the- if it's working. Posterior Sagittal Anorectoplasty. This is the new anus, the- posterior border, laterals, and the anterior border. Okay? We're now testing the function of the- look, the contraction of the- of the anus. Okay, it's working. Yes.
CHAPTER 9
I'm Paulo Castillo, pediatric surgeon in the Philippines as a volunteer in the World Surgical Foundation, Philippines. We did a 9 month old male who was diagnosed with an imperforate anus. This patient was born with imperforate anus high type and had an initial operation of a diversion colostomy, in which they did a divided sigmoid colostomy, and after which he was included, in the mission in the World Surgical Foundation, and we just did a posterior sagittal anorectoplasty. So we were able to identify the distal segment of the rectum, and we did a posterior sagittal anorectoplasty. For a patient with this- post-op- intra-operative- we were able to minimize bleeding, and we were able to dissect the distal segment with enough length and untwisted segment. Now, with our operation, we advise to maintain a Foley catheter for 3 days, and continue the antibiotic at least minimum of 5 days as well. So for daily wound care, it's always- we place an anal pack to- to control the hemostasis at the anoplasty, and we will remove that tomorrow, and then for the wound care, it's a regular care- wound care for the wound for a week. So dressing daily, antibiotics, hydration, and after which, after 2 weeks of the procedure, we will dilate the anoplasty by do- by placing a Hegar's dilator, size 13 and 14 for the appropriate age- size for the patient. We do that 2 times a day for at least 2 weeks. And once already dilated with the size 14 Hegar's dilator, we will subject the patient for the last- the third operation, after 6 weeks to 8 weeks in closing the, devine colostomy. So, we'll just wait for the patient to weight gain, adjust from our previous operation, and the complications of the procedure that we done is a stricture, infection, dehiscence of the anastomosis. So these are the possibilities of complications, that's why we always monitor the patient, to follow-up after a week for the wound care and then 2 weeks for the dilatation. And we regularly check the patient every 2 weeks, to check if there are any- first infection, strictures after 2 weeks, and possible if did not come back for a closure, possible stump closure. So, for that one, it's highly advised to the relatives to- to close follow-up. And then after 6 to 8 weeks, we can now close the- the colostomy. We can do that in a separate setting by doing just a single stage procedure, if it's caught on his first day. If it is a low type kind of imperforate anus, we could do outright posterior sagittal anorectoplasty without any diversion. If there- if the setup is complete, like you were in a tertiary hospital where available subspecialty doctors are there to support us, like the pediatric anesthesiologists, the neonatalogist, the pediatric surgeons of course, those are the set up for a tertiary hospital that we could do a primary procedure for the case.