Split-Thickness Skin Graft, Permanent Pigment Transfer, and Fractional CO2 Laser Therapy
Transcription
CHAPTER 1
Our first case today is a young child, 8 years of age. He is from Honduras originally, and at the age of 2, he was involved in a scald burn injury that was quite deep to his hand, his right hand, small areas of scarring to his right knee and his left hand.
I'm going to be doing some major work because of the burn contracture on his right hand. As he's grown, this has become tighter and tighter and made it look like almost a tendon abnormality, and it has impaired function related to that right hand. So we'll be releasing the scar, and the majority of that - it'll be such a large release, it'll require adding skin. So we'll be using a skin graft, and I believe I'll be using a split thickness skin graft technique where I'll harvest the skin from the thigh with a dermatome and then sew that into position with a graft to immobilize it, and then splint it.
The second part of that procedure - if there's some areas that require Z-plasty, may be accomplished at the same time on that hand, but I think he has a small area that bothers him - it's almost cosmetic, an area of burn dispigmentation, which is an area of hypo - almost vitiligo, it's very hypopigmented and it bothers him when he wear shorts. So we can make that better by permanent pigment transfer with the use of a small split thickness skin graft and dermabrasion. It permanently transfers a little bit of pigment to the area to camouflage the scar.
And finally, the third part of the procedure will be to try to soften the surrounding scar of the right hand and arm and the left hand with the use of a fractional laser. We'll use the laser system to basically create small little holes into the area of the scar where we can then use - rub in steroid into the area and it allows a little bit of remodeling of the scar that'll allow the scar to be a little bit softer.
At the completion of that, he'll have a splint on the right hand and have to be immobilized in that hand for 2 weeks before we take those dressings off. Burns heal by a combination of epithelization and contracture, and as he's continued to grow, he has a bad contracture across the dorsum of his hand. Make a fist? He can make a fist, but he gets a severe band contracture here. It's also hard for him to pull his thumb out all the way, so if we go ahead and release the contracture and add a skin graft, that'll allow him to move better. The tendons - just by having that contracture, makes it look like he has a tendon abnormality, but it's actually just the contracture that causes the abnormality of the motion of the finger. So if we treat the contracture, the motion of the hand will be - allow him to get his hand around a basketball when he's 18 years old, and allow the normal motion of the hand.
So I'll mark some areas where I'm going to make some incisions. So we'll make some incisions along here in the operating room. And that's where we'll be able to release and put in a graft. May also extend along there. He may also require a Z-plasty, so that'll take some of the tension by moving one direction to another. You borrow from one direction, and it lengthens it in the other direction.
So this is the contracture of the hand. It looks like there's a real problem with contracture along the region of the fingers, but in actuality, that skin, when you take the tension off, is normal, pretty much, with very little burn scar. So it's a contracture of the dorsum of the hand causing deformity of the fingers, as noted by the range of motion. It's a very difficult problem for him because of all this - these band contractures. These are skin problems, not tendon problems, so if you just release and treat the skin, it should treat the problem with the range of motion difficulties of the hand.
CHAPTER 2
Previous grafting looks good.
As you go through, you want to try to avoid going too deeply through scar into normal tissue. And fortunately there's a very good fat pad underneath the hand, which allows for a very good slide of tissue. If you're using very hypertrophic, early scar, you don't get this slide and you tend to have a cleavage into the normal tissues underneath the hand, causing a problem.
But already we can see that we have a very large defect. These are the standard veins you see on the dorsum of a normal hand that people can see and put in IVs into, so you can see it's a relatively superficial burn causing this significant contracture. We've gone through an area of previous skin grafting that was accomplished when he was a younger child.
We'll go up here, on top. Let's go through the first web space. Finger down. Thanks.
This is the first web space. There's a contracture in that area, as well. We're kind of just releasing it into the normal tissue on the palmar side, trying not to get into too much of the normal tissue or the palmar tissue, but with trying to fully release the contracture. Hold here, please.
So already we've got the thumb almost in a normal position. Still a little bit of contracture here. Just go another few millimeters into normal, trying not to get too much into the normal tissue but just enough to get the release that you need. There's still the band contracture along the ulnar side. Releasing it here, toward the normal. The more tension on the scar, the thicker that scar's going to be, so it's not surprising that this scar here looks to be 5 to 10 mm thick compared to some of the other scar because it was the one with the most tension on it.
Come on up for a sec.
Looks much better.
Yeah, boy. Could you flex the fingers down like that for me, please, and pull down?
Sometimes when the burn is very deep and has had a previous excision and graft, you're very quickly down to a pair of tenon and tendon, which makes it very difficult to get the slide you need to get a good result. Sometimes those patients require flap reconstruction instead of skin graft reconstruction, which is much more complex and requires a lot more postoperative therapy.
This bluish tinge, that would be the hypothenar musculature. In order to get the skin graft to take, it's going to require a very good hemostasis with very little bleeding underneath the graft and quite a bit of immobilization for about the 2 weeks that the stent that is going to be on there is going to be on. So we'll have to mobilize the fingers because too much motion of the fingers will decrease the ability for the - immobility of the graft that will be required.
Okay, I don't want to undermine too much. Now after all this undermining, you have to say, well, how much of that graft, that undermined skin, is that going to survive? Well, it's pretty close to what's there, so I think it will. Maybe a couple of edges that need to be trimmed back a little bit, but that's basically the release that we need. Some of this may secondarily require Z-plasty in the future. I'd rather not do that today because it may compromise some of the results of the skin graft, but it may require a staged approach of doing further Z-plasties along these abrasions.
I'd rather not get too much into the normal palmar skin because then you'd have a dark patch on his hand and if he raised his hand in school, there would be a dark patch and he'd be very embarrassed. So we'll try to avoid any dark patches on the - on the palmar side of his hand.
Do you have a ruler?
Sometimes in order to keep thing immobilized, we may K-wire the joints. I like to try to avoid K-wiring in children if we don't have to, basically because it can interfere - it can get infected or it can interfere with - growth plates - of the bones, and we want to make sure all those bones get to grow to their normal length.
So we'll go with a 4-inch shim on the dermatome. Epinephrine-soaked sponge. In order to decrease the bleeding postoperatively on the hand area, I'll put in an epinephrine-soaked sponge to decrease the bleeding, wrap that up while we concentrate on harvesting our skin graft.
Are you okay if we take it on the side? I think it'll be easier than -
Yeah, not from the previous side, but if you want to keep it above where his shorts line will be, so he doesn't have any scar problems with that.
Release the tourniquet.
CHAPTER 3
So I'm going to be moving for our skin graft portion of this. The harvest part. The electric dermatome is going to have a different sound than the air-driven one. Right here, if you see the shiny part of the 15 blade, that should just disappear when you check the thickness at 10 μm. It's at 10. It just disappears. It's just a way of helping calibrate what's already been calibrated. If you put it up higher, say at a 16, you'll fall all the way through. So that's how you know your specific calibration's going to work. And him, I think we'll push really hard at a 14 μm thickness to get a nice graft.
To decrease some of the postoperative bleeding and hopefully make the healing a little better, we'll do injection of diluted saline with a little bit of epinephrine in it. It also assists - that clysis assists in - harvesting the graft, especially in areas that are a little uneven, like, say, over the prominence of the hip. Along the area of the lateral thigh is one of the best donor sites, as it traverses along the femur. The long bone of the femur, it's very few irregularities so it's much easier to take a nice graft.
So, wipe off the previous Betadine. I like to use mineral oil to try to make it a little more slippery for the harvest. Oil on the dermatome. It's been measured out and will be the appropriate thickness we need.
I tend to go at about a 30 to 45 degree angle along the region that we need to take, pushing pretty hard along the way. And it always helps to have a great assistant. And then up like an airplane. There. And that's pretty evenly taken.
CHAPTER 4
So as we mentioned before, hemostasis in the region of the - the graft is going to be important in order to make sure the graft takes well. It's a nice vascular bed, so it will bleed a little bit.
Skin, please.
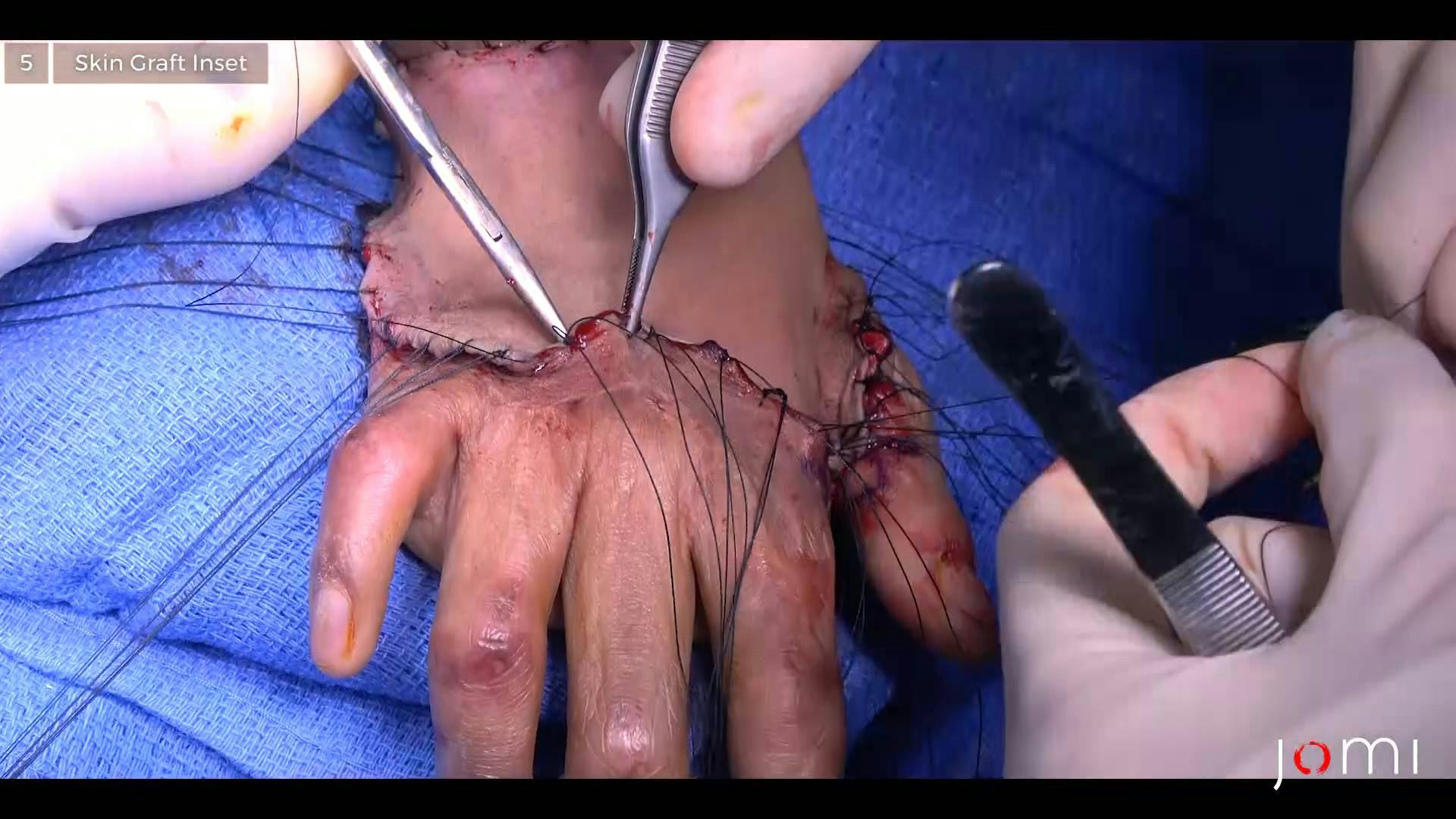
CHAPTER 5
Silks.
The skin graft, harvested at 14 in this young man, you can see it has quite a bit of dermis on it, means it's very white.
4-0 silk, please.
And it'll roll up a little bit. It has a little bit of primary contraction because it's got so much elastin it that it'll curl up a little bit at the edges. So that's about as thick a graft as you can take in a child this size, and the thicker the graft, the less post-secondary contracture that is likely to occur.
Let's start. Two multi-packs, please.
You want the empties here?
Do you have a finer Adson?
Multipack.
Finer Adson.
Thanks.
If you feel it's a little on the oozier side, you can do some pie-crusting to the area. Pie-crusting will allow a little bit of the blood to drain so that you're not going to get bleeding under the graft, which will decrease the chances of it taking postop. The most common places for a little bit of blood pooling would be the corners, so maybe we'll do a little pie-crusting in the corners if we have any issues. Sometimes when you take the tourniquet down, there's a little bit of hyperemia from the previous ischemia to the hand because of the tourniquet, so sometimes you get a little bit more bleeding than you might expect. You just have to be patient and wait for that post-tourniquet hyperemia to kind of abate.
And just put it in as much as you can. Like that.
I just don't want it to roll up.
Yeah, I get that. I'm going to need every bit of it.
It's just curling a little bit.
Yeah, and sometimes if it curls a bit, you can do a half-mattress on the corner to try to suck it right into that edge of the - the suture line that you've got.
Can I have a SNaP, please?
I like to put as much as dermis as I can in there and that helps decrease the secondary contracture. The more - The more you put in, the less stuff contractures. So there will be a sense of - there will be raised edges on either side in the immediate postoperative period. That sometimes alarms the patients a bit, but we do a lot of therapy postoperatively to decrease the secondary contracture where the - where it tries to pull in and get smaller again.
This kid's very compliant, so I don't think I have to do anything with immobilizing the fingers with pinning, with K wires. But that is an option to consider, especially if there's a lot of work that has to be done on the MCP joints, metacarpophalangeal joints.
SNaP will be next.
SNaP.
Any areas where we have excess?
No, there's not a lot of…
You've got the tough corner, don't you?
Yeah, but it looks - I mean, we can put - Do you want more in the web space, maybe? Because it seems - I mean -
No, it looks good. You might need a couple more silks in there, if that's what you mean - maybe 1 or 2 extras.
We're going to irrigate onto the graft at some point, too.
May I have some SNaPs, please?
Another SNaP.
Another silk.
I usually like to sew them in from the skin graft to the hand side, just makes it a little easier to sew in. Trying to sew from the the normal hand side to the skin graft tends to be a little harder to get as much accuracy.
SNaP.
May I have the Stevens scissors, please?
SNaP.
You want a silk?
No, a SNaP.
Drill a couple little drain holes, just in case there's a little bit of bleeding. Hopefully it won't accumulate much and we can get nice healing.
Little irrigation underneath.
Do we have xeroform?
Yes.
CHAPTER 6
So we got a good look, there's no real significant bleeding underneath there. The little compression from the stent itself will be helpful in trying to decrease the - any oozing that tries to happen underneath the graft.
Do we have the cotton?
Heavy scissors, please.
Do you have an empty needle driver?
Some people put mineral oil on this or moisten it. I tend to go with the dry cotton. It's just dealer's choice, doesn't really matter too much, I don't think. I do tend to use a fair amount of cotton, maybe more than most, but - Everybody kind of finds what's perfect for them and what works for them the best.
Okay, sloppiest of sloppy wets, please.
So all these little silks are going to be tied across this dressing, and then - it'll immobilize it and then we'll splint the fingers. I think I'll go with this one. In 2 weeks, this dressing will come down and we'll see how good our graft take is, if there's any problems with fevers or the stent is moving or there's a lot of bleeding, then of course that'd be - we'd take it down early to make sure everything's okay, but in general, when you have a surgically-created wound - a little - try it again, please - surgically-created, um - release, it's relatively a sterile wound, so you don't have to worry about infection as much as you would for, for instance, a - a contaminated open wound, when you're grafting a contaminated open wound.
I'll take those two together and get this funky corner done. Let's see - let's go with one of those. Split the difference.
Let's see what we've got here. I'll have you bring the fingers down just a little bit, like that.
We used a Webster needle driver that has very little tread on it so it's less likely to break the silks as we're tying them down. So if you kind of hold it with a regular needle driver, like that, when you try to release it after the knot, it can sometimes break the stitch.
Heavy scissors.
Could I have a sponge, please? I'm going to want some sponges, unclipped sponges for the fingers, and then we'll wrap with a cling.
Do you want OT?
Yeah, we'll call for them, but then we're going to - we'll just take the small skin graft off on the - for the knee and the dermabrasion, have you seen that procedure yet? I'll show you.
Do you have a cling?
Yes.
Oh, perfect, thank you.
So again, not too tight, but snug. Kind of bend the MCPs a little bit.
Now we're going to take a little bitty piece of skin graft for the knee. So we're doing a dressing where we can see all the fingertips and thumb tip but we'll then splint it with a - a splint decreasing the range of motion of - well, wrist down to MCPs, so - there may be some motion to the PIPs, but the MCPs will be immobilized in that position and the thumb is immobilized, so, the immobilization is greatly helpful. For the graft to take, immobilization is required.
CHAPTER 7
So we can permanently transfer pigment to that dark spot just by the smallest of skin grafts. We just take a little bitty piece next to the one we have already and then add it there, and it'll permanently transfer the pigment so that it'll match a little bit better and he'll be less embarrassed when he's playing soccer.
A little better lighting on that area of dispigmentation.
This usually happens in areas of pretty deep burn where the pigment doesn't recover. Most pigments will recover within 6 months to a year, especially in dark-skinned people, but this one didn't, so it's clearly because it was much deeper burned, more deeply injured.
The dermabrader is the way we kind of take off the top layer of the skin here. So you just put it on the skin and just take the top layer off.
Could we have some gauze, please?
And that's about it. So the dermabrader's nice, all it requires is just taking the top layer off. I'll just take the smallest of small skin grafts here at a much thinner rate, maybe 8 μm instead of the 14. Put it down to 8. Just squeeze like that.
So, push on both sides. I already put it on, thanks. Push on your side with me. I'll push on this side, you put it on that side.
Nice. Do you have an epi-soaked sponge?
So here we have just a very small skin graft that we'll put right on here to transfer that pigment, make it a little darker. This one is much thinner than the last one, it'll have much less white than the last one did, because it's mostly just an epidermal graft with very little dermis. Because you don't need the dermis if you're just transferring pigment.
Will you need silk for that?
No, we're going to use Histoacryl.
Okay.
So it's such a small graft and very thin, it's kind of hard to sew in. We'll have to do a little needle mobilization to make sure the graft takes, but you can take a little bit of cyanoacrylate, or whatever you want to call it, Dermabond or Histoacryl. I'm doing what some of these guys call spot-weld, you kind of fix it in a couple spots, and then you're done.
So you just wrap the knee and immobilize it, and it should take as a graft. If it did take completely, it should heal up very well and eventually that pigment - looks like a little bit of a patch, like a stamp of darker skin in the area, but then that fades and turns into being very similar to the surrounding color and it's much less conspicuous. And since he already has his large donor site to recover from, this little bit extra is pretty minimal.
I'll take a little square of xeroform, please.
For the donor site, we inject a lot of local anesthetic into the donor site because this is what's going to hurt the most. And we can even do a lateral femoral cutaneous nerve block, whether with ultrasound or just by landmarks. And we'll do a xeroform followed by a Telfa followed by a dry gauze wrap, and that'll come down tomorrow.
CHAPTER 8
Do you want chromic?
I think we don't need it because it's going to be pretty immobilized just by the dressings.
So a little bit near the lateral femoral cutaneous nerve as it runs out underneath the inguinal ligament on top of the Sartorius, traversing down toward where this donor site is, and then to get some of the twigs as they get into the area of the donor site. Twigs of nerves. And then anesthetize - the donor site as much as we can for the amount of local we can use. We stop at about a cc per kilo of 0.25 marcaine with adrenaline.
I'm going to take what we have left and give like a dorsal wrist block.
So we're done except for laser, right? So I can start breaking sterility. I'll take a Kerlix, please.
Do you have a stapler? Could I have it, please? Thanks.
In order to tell some people, 'don't take this dressing off,' we'll sometimes put staples across it as a reminder that this isn't the donor site, it's the graft site. But they can take this dressing down tomorrow. We usually keep most of our skin graft patients in the hospital overnight to make sure they have good pain control.
CHAPTER 9
So, dorsal hand release - pretty good-sized graft, need to immobilize kind of the MCPs, that's kind of where it needs to be. The MCPs are about 70°, and thumb. I don't want the wrist or the MCPs to move, I think - the graft's here, so whatever you think is -
I might do Bohler, just because -
Okay.
- it's harder to flex against it when it's…
Sounds good. Bohler splint will be perfect. Yep. Thanks.
And his knee would need an immobilizer, or a knee extensor.
A prefab knee immobilizer will probably work.
Alright.
Thank you. Probably a small adult.
CHAPTER 10
Alright, so, we're going to do a little laser on this burn scar on the back of his hand. It's a little hypertrophic, it's not too bad. And then we're going to work a little bit on his left hand.
I think some of the key things to think about is laser safety. We've got the air handler going, which can be a bit loud, but we've got our stent from our surgery, we want to cover that up because that's flammable. And then behind him, this is a wet drape as well. So these two things will decrease - will help improve laser safety. The laser itself, we're just going to be doing a deep today - sometimes you can do a CPG or superficial treatment - and then - but in this case, I think we just want to do just the one laser for him. It tends to soften up the scar and make it a little better.
We always do a test to see that we have it correctly, everybody around us all has goggles on. And then if you can get a close-up of that, you can see how there's a square pattern, and that pattern - it has bunch of little holes in it. So this is a fraxel laser that treats very deeply, but only a small percentage of the skin is treated at a time. The higher the energy, the deeper it goes, but then you have to decrease the density. In this case, it's quite safe to go ahead on this relatively minor scar, 25 mJ and a 10% density. If it was very hypertrophic, I would consider going up to perhaps a SCAAR FX at 100 mJ, or even more, at about a 3% density.
It's got a foot pedal to help control it.
We use different topical agents after it's done. We've got all these micropores placed into the skin, so we feel that if we then massage in a little bit of Kenalog, triamcinolone steroid, that may help soften up the scar as well. I've been using a little betamethasone for - instead of Aquaphor or Vaseline gauze, but that is a separate choice depending on what you want.
So now we're going to concentrate on his left hand.
Kenalog.
So the next thing we like to do is rub in a little Kenalog into these little pores. So all these multiple little pores, we've got Kenalog, 10 mg per cc. I'll just drip a little bit on there, I've got sterile gloves on. It's a clean procedure, not sterile, but I like to make sure we can minimize any potential postcellulitis, which is pretty uncommon.
Rub a little of that Kenalog in. And then we'll put on the dressings. A little bit up here.
These are not very hypertrophic scars, but they will get a little softer with this. And, um - the children always seem to think that there's an improvement and are very happy to have additional procedures, which is pretty uncommon for kids to want procedures.
I've been just trying a little bit of a betamethasone.
You can just give it to me, thanks. Perfect.
So the betamethasone ointment, just put a little bit of that into the - That's just a personal preference, it's - everybody's got a little bit of different personal preferences. And then we'll put Vaseline gauze dressing on there for 5 days.
And that's it. Great. Thanks, I'll let you work your magic with the dressings.
CHAPTER 11
So in the first case, we were able to harvest a skin - get a tremendous release in the dorsum of the child's hand, on the right hand. The entire contracture causing all that tightness was ameliorated by a release down to the level of the subcutaneous tissue, but not into the fat. It released very quickly. We had an 8 by 8 cm defect without excising any scar or previous skin grafts harvested the skin graft from the thigh, sutured into position with a good immobilization. No Z-plasty seemed to be warranted, or didn't seem to be warranted at this time; secondarily, they may be warranted.
The second part of his procedure was a grafting to a small area of dispigmentation on his knee with a small skin graft and immobilized there, that worked out well. And finally the third procedure, we did some - just as we had intended, some laser to the area of his bilateral upper extremities. And some steroid was rubbed into the area of the wound, so hopefully that'll affect a softer scar for him. He will be immobilized for 2 weeks and we'll get a better idea of how the skin graft has taken and his improvement in function will be after 2 weeks' time.