Ulnar Nerve Transposition (Cadaver)
Main Text
Table of Contents
Ulnar nerve transposition is a surgical procedure performed to treat ulnar nerve compression of the elbow, also known as cubital tunnel syndrome. This procedure is utilized after both non-operative management and in situ decompression fails, or if these procedures are deemed inappropriate based on patient pathology or ulnar nerve instability. Transposition of the ulnar nerve involves not only decompression of the nerve but also its anterior repositioning to reduce compression and irritation while maintaining nerve integrity. This video demonstrates, on a cadaver arm, the operative technique for performing an ulnar nerve transposition using either a subcutaneous or a submuscular technique.
A 55-year-old male presents to you with sensitivity in his right elbow. He reports that the pain occurs on the posteromedial aspect of the elbow, and it is particularly bad when he flexes his elbow, such as when he is using his cell phone. He describes the feeling as a 5 out of 10 “aching” pain and says that it is sometimes accompanied by a sharp tingling sensation in his little finger and ring finger. He is also concerned because he feels his right-hand grip has recently become weaker. The patient’s past medical history is significant for an in situ cubital release performed on the right elbow 1 year prior for treatment of similar symptoms. The patient states he is particularly frustrated because the pain often wakes him up at night if he bends his arm in his sleep, and he cannot get a decent night’s sleep.
Cubital tunnel syndrome is seen with a slightly higher incidence in males than females, and increasing incidence is seen with increasing age in both genders.1 Individuals that perform repetitive or prolonged activities requiring the elbow to be in a fixed bent position are at an increased risk for developing cubital tunnel syndrome.2
Physical exam findings will vary based on the etiology and severity of the nerve compression. When the arm is moved through a full range of flexion and extension, the ulnar nerve may be observed subluxing over the medial epicondyle. There may be visible muscle atrophy of the affected hand around the little finger and ring finger, as well as clawing. This can be accompanied by decreased sensation in these fingers. Swelling and/or a cyst may be observed by the medial epicondyle.3 A positive Froment’s sign, indicating a compensatory thumb flexion during a pinching motion, is characteristic of ulnar compression. Additionally, persistent little finger extension and abduction, known as a positive Wartenberg’s sign, suggests ulnar nerve compression. Motor testing that reveals a weakened grasp and/or pinch also supports this diagnosis.3,4
Cubital tunnel syndrome is due to compression and irritation of the ulnar nerve at the elbow by the medial epicondyle. The cubital tunnel is a narrow space that the nerve must traverse with very little surrounding soft tissue for protection. Often, the exact cause of this nerve irritation is not known, but causes include holding a phone to the ear extensively, leaning on the elbows, an elbow cyst, and elbow arthritis. If the ulnar nerve remains compressed for an extended period of time it can lead to irreversible muscle wasting in the hand as well as ongoing pain and decreased function of the affected elbow and hand. For patients presenting with mild or moderate nerve compression, first-line treatment involves discontinuing activities that increase nerve compression, taking NSAIDs, and wearing a padded elbow brace or splint. If the nerve is severely compressed or non-surgical treatment methods are ineffective, then surgery is indicated. Surgical procedures include cubital tunnel release and anterior nerve transposition.3
X-ray can be used to visualize the bony structure of the elbow and reveal any bone spur or arthritis that may be responsible for the nerve compression. Nerve conduction studies are useful in determining the condition of the ulnar nerve, where the compression is occurring, and whether or not there is any associated muscle damage.
This procedure is performed under general or regional anesthesia using a sterile tourniquet. Position the patient supine with the arm externally rotated and flexed slightly so that the posteromedial aspect of the elbow is exposed. Disinfect the incision site, then fully extend the elbow and palpate the medial epicondyle to locate the ulnar nerve. Mark out the location of the ulnar nerve posterior to the medial epicondyle, extending 6–10 cm in both the proximal and distal directions.
Flex the arm slightly to visualize the path of the nerve. Create a longitudinal incision directly behind the medial epicondyle along the marked path. Dissect proximally to the medial epicondyle, down through the subcutaneous tissue. Open the incision and cauterize blood vessels as necessary. Identify the ulnar nerve proximal to the medial epicondyle.
Release the proximal ulnar nerve arcade using a spreading motion with scissors. Push the nerve around as needed to perform the release, but avoid grabbing it to prevent damage to the nerve or its accompanying blood vessels. Confirm the nerve is mobilized. Continue making a longitudinal incision distal to the medial epicondyle, and confirm the nerve is mobilized. Insert retractors at both the proximal and distal ends of the incision. Release the distal ulnar nerve arcade and confirm the nerve is mobilized. Take care to avoid cutting through any nerve branches or vessels. If one of these structures is inadvertently cut, be sure to cauterize it to prevent painful neuromas or excessive bleeding. Release the fascia between the 2 heads of the flexor carpi ulnaris (FCU), making sure to release the fascia in line with the nerve. Check for any deep investing fascia, and if any is observed, spread the fascia with scissors to release. Once the cubital tunnel has been fully opened and the ulnar nerve mobilized, gently pull the ulnar nerve away from the released fascia. Maintain the branches from the ulnar nerve if at all possible, and cauterize any nerve branches that cannot be preserved.
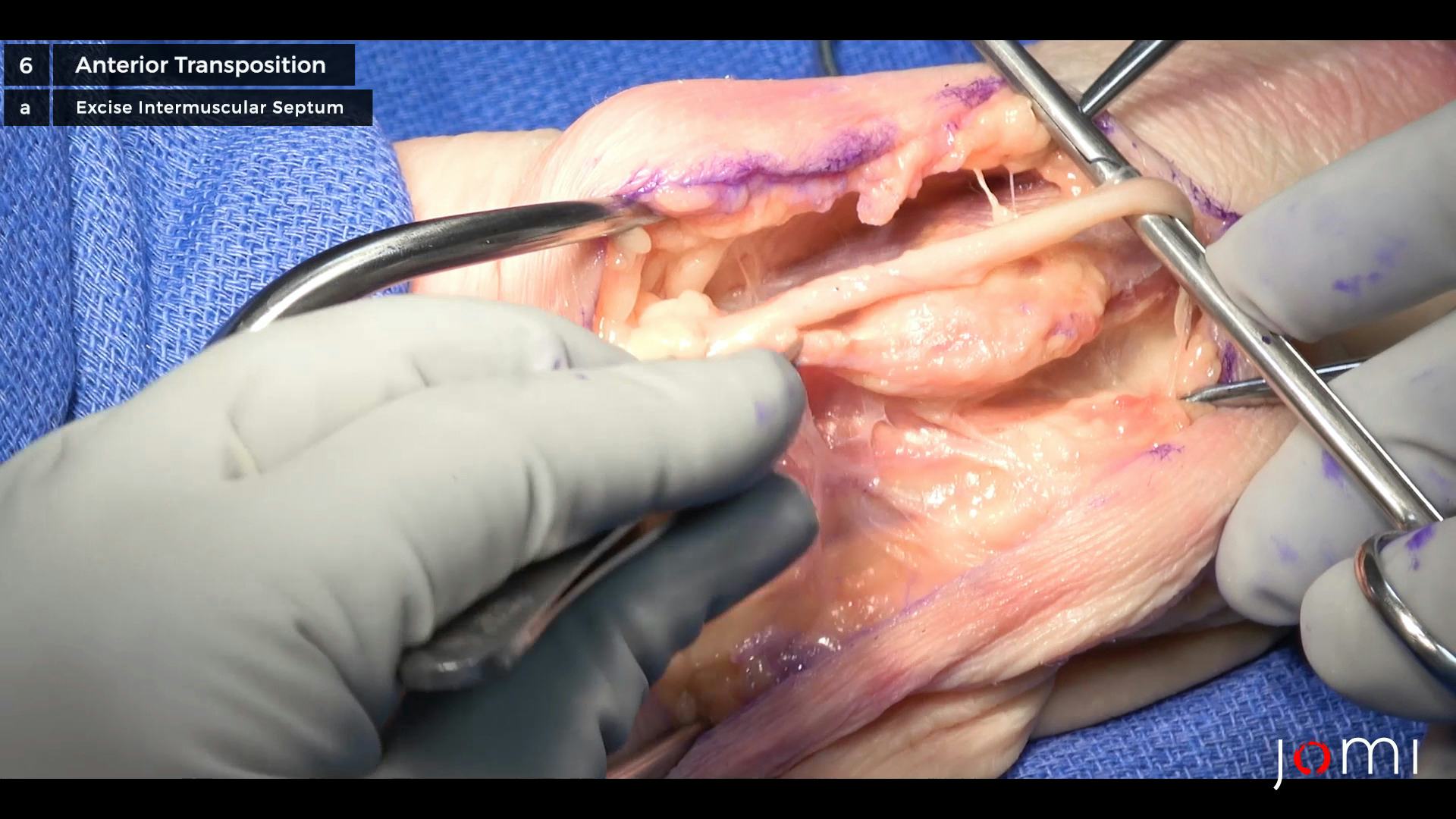
Once the nerve is mobilized, remove the intermuscular septum from the medial epicondyle using either a knife or a cautery. Excise about a 1-cm segment so that there is a bare supracondylar ridge exposed. Take care to protect the motor nerve branch on the ulnar side of the septum. Reposition the nerve by moving it anterior so that it sits over the supracondylar ridge without interference from any external structures. Cauterize the first branch of the ulnar nerve if it is tethering the nerve and inhibiting anterior mobilization and transposition.
Subcutaneous Technique. Close the cubital tunnel to prevent inadvertent resubluxation. To do this, mobilize the posterior tissues from the triceps extension and close the tissue flaps across the interval enclosing the medial epicondyle. Apply 2 figure-of-eight sutures to complete the closure. Then create a fascial sling to hold the nerve in place anteriorly. This can be done by repositioning the posterior aspect of the FCU across the nerve, leaving the fascia attached to its origin on the epicondyle. Use a 2-0 Vicryl or equivalent to fix the sling.
Submuscular Technique with Z-plasty. Temporarily translate the nerve posteriorly. Incise the flexor pronator muscle belly in a Z-fashion to create leaflets. To do this, mark out flaps on the flexor pronator muscle origin using three parallel lines: one on the leading edge, one down the middle, and one where you decompressed the ulnar nerve. This will create a distal flap and a proximal flap. The distal flap requires some dissection off the muscle, but the proximal flap pulls off rather easily because it goes in the direction of the muscle fibers. Move the nerve to within the prepared flexor pronator muscle leaflets. Connect the muscle leaflets end to end with 1–2 figure-of-eight sutures. Take care not to stitch too tightly, or there is a risk of inadvertently creating a new site of constriction on the nerve.
Now that the nerve has been stabilized, take the nerve through an active range of motion. Release any residual tension resulting from deep investing fascia.
Wash the wound thoroughly with sterile water. Drop the tourniquet. There may be a moderate amount of bleeding, so cauterize as needed. Close the skin with 3-0 Vicryl, a running 4-0 Monocryl, and then a glue or nylon for the skin.
Apply a cast or splint to the elbow to maintain a 90° bent position for 2–4 weeks postoperatively. Physical therapy is recommended to regain strength and range of motion, as well as to help with pain management.
Ulnar nerve transposition is considered an effective long-term treatment option for patients with cubital tunnel syndrome. It is most often recommended in cases where simple in situ cubital tunnel release is contraindicated,3,5–9 such as in cases of prior elbow trauma or underlying pathology.10 Retrospective studies have shown that in patients without elbow arthritis or elbow trauma, in situ decompression is an effective option for treating cubital tunnel syndrome that carries lower risk of adverse events and recurrence than ulnar nerve transposition procedures.7,9 A 2018 prospective cohort study found that patients experienced greater surgical morbidity following ulnar transposition than decompression as measured by narcotics consumption, patient-reported disability, and persistent olecranon paresthesia. However, most of these differences were transient and resolved by 8 weeks after surgery.5
A meta-analysis of four randomized controlled trials found no difference in motor nerve-conduction velocities or clinical outcome scores between simple decompression and ulnar nerve transposition in patients without prior traumatic injuries or surgeries of the affected elbow.6 A 2015 cadaveric study showed that both subcutaneous and submuscular transposition provided a statistically significant decrease in nerve strain in full flexion, while in situ release did not provide a change in strain in either flexion or extension. These results provide evidence that an ulnar transposition may be warranted over an in situ release when strain is the underlying pathology causing ulnar neuropathy.8
Once a surgeon has deemed a patient to be an appropriate candidate for ulnar transposition, there are a few transposition techniques to choose from. The current literature provides limited insight into the different outcomes between the available techniques. A 2015 meta-analysis of the available randomized controlled trials and observational studies comparing subcutaneous and submuscular transposition techniques found no difference in the outcome of clinically relevant improvement. However, the authors found that the incidence of adverse events was significantly higher following submuscular transposition than subcutaneous transposition. The authors acknowledged that the outcomes used in the various studies were inconsistent and there were very few randomized controlled trials, so more evidence is needed on this topic in order to draw meaningful conclusions.11 Retrospective studies have found similar evidence that while both subcutaneous and submuscular transpositions effectively treat cubital tunnel syndrome, submuscular transposition is associated with higher recurrence and more complications.12,13
Nothing to disclose.
The patient referred to in this video article has given their informed consent to be filmed and is aware that information and images will be published online.
Citations
- Osei DA, Groves AP, Bommarito K, Ray WZ. Cubital tunnel syndrome: incidence and demographics in a national administrative database. Neurosurgery. 2017;80(3):417-420. doi:10.1093/neuros/nyw061.
- Adkinson JM, Zhong L, Aliu O, Chung KC. Surgical treatment of cubital tunnel syndrome: trends and the influence of patient and surgeon characteristics. J Hand Surg Am. 2015;40(9):1824-1831. doi:10.1016/j.jhsa.2015.05.009.
- Grandizio LC, Maschke S, Evans PJ. The management of persistent and recurrent cubital tunnel syndrome. J Hand Surg Am. 2018;43(10):933-940. doi:10.1016/j.jhsa.2018.03.057.
- Goldman SB, Brininger TL, Schrader JW, Curtis R, Koceja DM. Analysis of clinical motor testing for adult patients with diagnosed ulnar neuropathy at the elbow. Arch Phys Med Rehabil. 2009;90(11):1846-1852. doi:10.1016/j.apmr.2009.06.007.
- Staples R, London DA, Dardas AZ, Goldfarb CA, Calfee RP. Comparative morbidity of cubital tunnel surgeries: a prospective cohort study. J Hand Surg Am. 2018;43(3):207-213. doi:10.1016/j.jhsa.2017.10.033.
- Zlowodzki M, Chan S, Bhandari M, Kalliainen L, Schubert W. Anterior transposition compared with simple decompression for treatment of cubital tunnel syndrome: a meta-analysis of randomized, controlled trials. J Bone Joint Surg Am. 2007;89(12):2591-2598. doi:10.2106/JBJS.G.00183.
- Zhang D, Earp BE, Blazar P. Rates of complications and secondary surgeries after in situ cubital tunnel release compared with ulnar nerve transposition: a retrospective review. J Hand Surg Am. 2017;42(4):294.e1-294.e5. doi:10.1016/j.jhsa.2017.01.020.
- Mitchell J, Dunn JC, Kusnezov N, et al. The effect of operative technique on ulnar nerve strain following surgery for cubital tunnel syndrome. Hand (NY). 2015;10(4):707-711. doi:10.1007/s11552-015-9770-y.
- Gaspar MP, Kane PM, Putthiwara D, Jacoby SM, Osterman AL. Predicting revision following in situ ulnar nerve decompression for patients with idiopathic cubital tunnel syndrome. J Hand Surg Am. 2016;41(3):427-435. doi:10.1016/j.jhsa.2015.12.012.
- Krogue JD, Aleem AW, Osei DA, Goldfarb CA, Calfee RP. Predictors of surgical revision after in situ decompression of the ulnar nerve. J Shoulder Elbow Surg. 2015;24(4):634-639. doi:10.1016/j.jse.2014.12.015.
- Liu CH, Wu SQ, Ke XB, et al. Subcutaneous versus submuscular anterior transposition of the ulnar nerve for cubital tunnel syndrome: a systematic review and meta-analysis of randomized controlled trials and observational studies. Medicine (Baltimore). 2015;94(29):e1207. doi:10.1097/MD.0000000000001207.
- Bacle G, Marteau E, Freslon M, et al. Cubital tunnel syndrome: comparative results of a multicenter study of 4 surgical techniques with a mean follow-up of 92 months. Orthop Traumatol Surg Res. 2014;100(4)(suppl):S205-S208. doi:10.1016/j.otsr.2014.03.009.
- Zhou Y, Feng F, Qu X, et al. [Effectiveness comparison between two different methods of anterior transposition of the ulnar nerve in treatment of cubital tunnel syndrome]. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2012;26(4):429-432. http://open.oriprobe.com/articles/29148370/EFFECTIVENESS_COMPARISON_BETWEEN_TWO_DIFFERENT_MET.htm.
Cite this article
Kalbian I, Ilyas AM. Ulnar nerve transposition (cadaver). J Med Insight. 2023;2023(206.5). doi:10.24296/jomi/206.5.