De Quervain's Release (Cadaver)
Main Text
Table of Contents
De Quervain’s release is a surgical procedure performed to curatively treat stenosing extensor tenosynovitis of the first extensor compartment of the wrist after nonoperative management fails. This procedure involves surgical release of the first dorsal compartment with care taken to fully release the abductor pollicis longus (APL) and extensor pollicis brevis (EPB) tendons from their respective sheaths, while protecting the radial sensory nerve, in order to decompress the extensor tendons. This video outlines the operative technique used by Dr. Asif Ilyas for performing a De Quervain’s release on a cadaveric wrist.
A 44-year-old female presents to you with pain in her right wrist. She reports that she spends about 2 hours each day working in her gardens using her hands, and she is right-handed. She complains that her symptoms include pain on the radial aspect of the right wrist that sometimes travels up her right forearm. This pain has become gradually worse to the point that she now rates it at a 6 out of 10, and she states that the pain is worse if she is using her thumb and wrist, especially with any kind of grasping motion like holding a shovel. The patient tells you that she is also disturbed by a painful snapping sensation that she feels periodically during daily activities on the radial aspect of her wrist.
De Quervain’s tenosynovitis (also known as De Quervain’s syndrome) is more commonly seen in women than men, and most often occurs in the wrist of the dominant hand. The greatest incidence is seen between the ages of 30–50.1 It is associated with overuse due to repetitive and/or forceful motions as well as trauma to the thumb or first dorsal compartment.2 Postpartum mothers and individuals providing infant care are a subset of De Quervain’s patients who tend to be younger and suffer due to repeatedly lifting infants throughout their day.3
Tenderness over the first dorsal compartment is usually observed, and there may also be swelling in this area. A fluid-filled cyst may be palpated in the region of the swelling. Pain is elicited with resisted radial wrist movement. There is no gold standard diagnostic test; however, the Finkelstein maneuver is positive in typical cases and has been shown to have an inter-observer repeatability of 0.79.4 The Finkelstein maneuver involves holding the patient’s thumb and abducting it towards the ulna; if this movement increases pain in the radial styloid and along the path of the adductor pollicis longus (APL) and extensor pollicis brevis (EPB) tendons it is considered a positive test.4
De Quervain’s tenosynovitis is believed to be caused by thickening of the APL and EPB tendon sheath due to degenerative changes like mucopolysaccharide deposition and myxoid tissue degeneration, as opposed to an inflammatory reaction.5 This thickening of the retinaculum impairs the normal movement of the APL and EBP tendons leading to wrist pain and impaired wrist movement.6 If left untreated the pain will become progressively worse and wrist function will decrease. Conservative management consisting of corticosteroid injection into the first compartment along with rest and immobilization is the first-line treatment option. The reported success rate for corticosteroid injection ranges from 62–80% with up to two injections administered properly into the tendon sheath.3, 79 Patients who fail conservative treatment may require surgical release to open the tendon sheath and relieve pressure on the tendon. The most common reason for injections to fail is missing the compartment and/or the presence of subcompartments.
On plain x-ray, AP and lateral views of the wrist may show non-specific signs like swelling over the radial styloid, and these views can be used to rule out conditions like fracture or carpal arthritis. Ultrasound can be used as a diagnostic tool and important findings include thickening of the first dorsal compartment retinaculum, edematous thickening of the APL and EPB tendons, and increased fluid within the first compartment sheath.10 MRI is highly sensitive and can pick up tenosynovitis and tendinosis findings beyond the capabilities of ultrasound. MRI can also be used to evaluate if there is an EPB subcompartment.11
This procedure can be performed under local anesthesia with the patient awake, or it can also be performed under sedation and/or regional anesthesia. The patient is positioned supine with the arm of interest outstretched laterally, supine, and supported by an armrest.
Begin by marking out the path of the APL and EPB tendons on the wrist to provide a visual of the tendon path. Mark your incision site over the first extensor compartment just distal to the radial styloid. Inject the incision site with a local anesthetic, and have the patient confirm lack of feeling in the surgical site after injection to ensure sufficient analgesia is achieved.
The incision can be made longitudinally, obliquely, or transversely. A longitudinal or oblique cut will decrease the chance of inadvertently injuring the radial sensory nerve. Keep this incision shallow initially, cutting only through the epidermis and dermis and preserving the subcutaneous tissue to avoid inadvertent damage to the radial sensory nerve. Once you have exposed the subcutaneous tissue, begin bluntly dissecting down to the first compartment by spreading the subcutaneous tissue longitudinally with your scissors. As you spread the tissue, identify the radial sensory nerve branches and carefully retract them. The nerve branches must be carefully protected and retracted throughout the procedure to avoid nerve injury. Insert right angle retractors to keep the incision open and to keep the nerve branches out of the surgical field.
With the superficial dissection of the first compartment completed, the tendons should be visible within their sheath. The release should be performed longitudinally in line with the tendons, along their dorsal border. Begin the release using a scalpel to open the retinaculum incrementally. Releasing the tendon incrementally will allow you to confirm protection of the nerve branches throughout the release. Perform the release along the dorsal border of the retinaculum to decrease risk of postoperative tendon subluxation. Once the sheath is fully released in the proximal direction, repeat the release along the dorsal border distally.
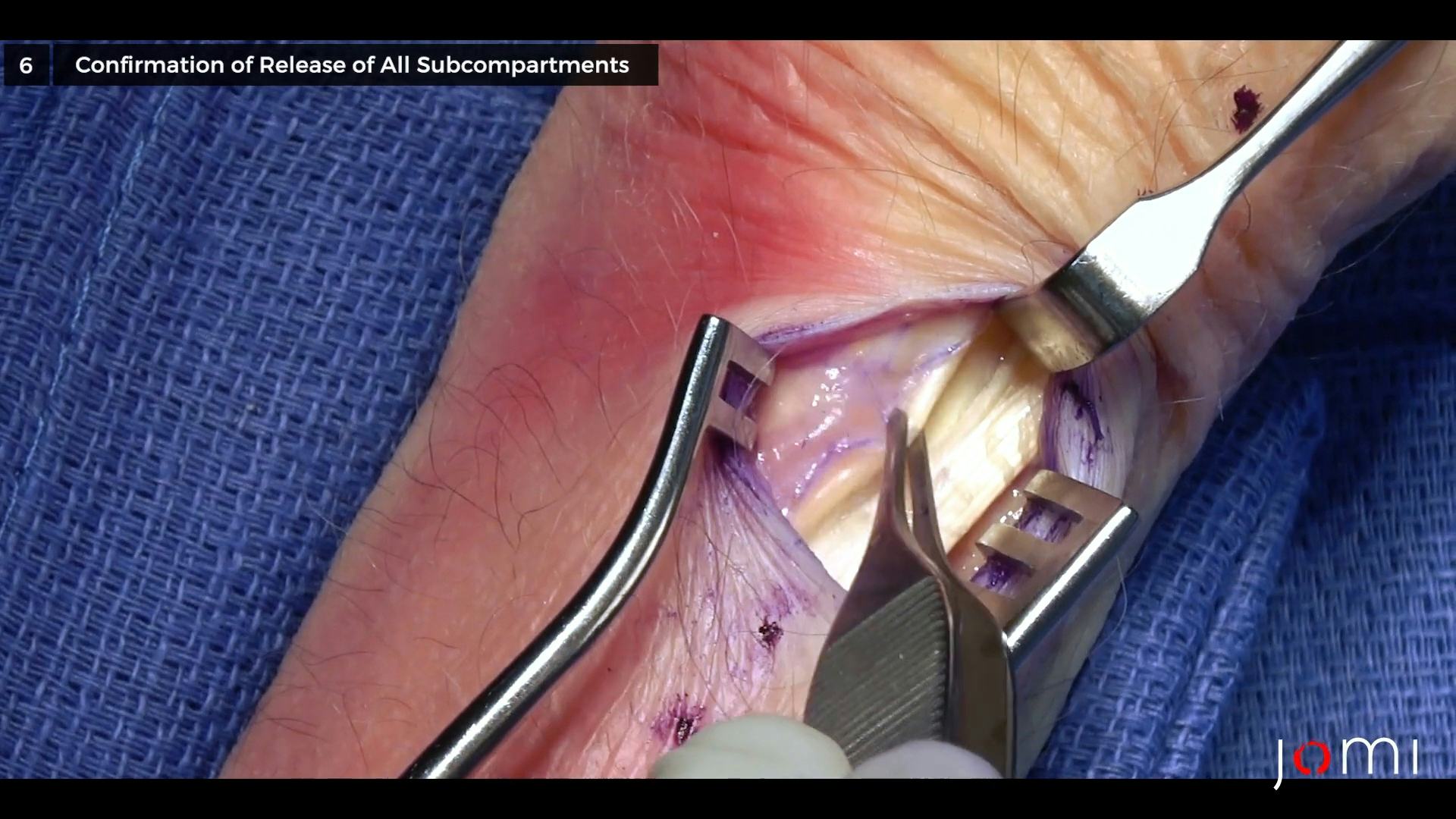
Both the APL and EPB tendons should now be clearly visible, with the APL tendon being larger and volar, and with the EPB tendon being smaller and dorsal. Examine both tendons carefully for subcompartments that may also need to be released. Although you have decompressed the first compartment, these tendons may have multiple slips, with the EPB often residing within its own subsheath. If you identify a subcompartment, repeat the longitudinal release. Confirmation of complete release can be obtained by pulling the tendons out of the wound with retractors. Once all subcompartments have been released, check that the compartment floor is clear of any additional synovitis so that you can only see the radius and the insertion of the brachialis tendon. Tenotomy scissors can be used to help mobilize the tendons if needed, and they can also be used to release any remaining adhesions and debride additional tenosynovitis that may be observed in the compartment. If your patient is awake, instruct them to move their thumb to confirm the compartment release. Remove the retractors and examine the radial nerve branches again to make sure they are fully intact prior to closing the incision.
Wash the wound thoroughly with sterile water. Ask the patient to move their wrist to once again confirm complete release as well as to make sure there is no tendon subluxation. Close the wound with suture while taking care to examine the radial sensory nerve with each throw to avoid placing a stitch in a radial sensory nerve branch. Apply a bulky soft dressing over the closed wound.
Patients should wear the soft dressing for at least 2–3 days, taking care to keep the dressing dry. The use of a protective splint is recommended. Patients return for suture removal after 10–14 days. Therapy is occasionally needed and recommended on an as-needed basis.
De Quervain’s release is considered an effective long-term treatment for stenosing tenosynovitis of the first compartment after conservative treatment has failed, with patient satisfaction ranging from 88–100%.12–14 A 2008 study of 94 consecutive De Quervain’s procedures identified only 6 cases of postoperative complications, and 100% of patients reported absence of pain and triggering both subjectively and upon examination at a 10-year follow-up.12 Another study of 43 consecutive procedures found that at 3-year follow-up the cure rate, defined as no postoperative complications, was 91% with 88% of patients indicating they were fully satisfied.13
Patient-reported dissatisfaction has been found to be significantly associated with long-term complications after De Quervain’s surgery. Significant complications include incomplete release of tendon subcompartments, tendon subluxation, and radial nerve damage.14 Scheller et al.1 found that out of 94 cases there were 6 complications including 1 superficial wound healing, 1 delayed healing, and 4 transient radial nerve lesions. When 43 consecutive cases were examined at an average of 3-year follow-up, there were 2 patients with recurrence of De Quervain’s tenosynovitis (5%), 1 radial sensory nerve injury (2%), and 1 severe scar tenderness (2%).2
Although further research is needed to gain more insight regarding incidence of complications following De Quervain’s release, there are evidence-based suggestions that surgeons can follow to decrease the risk of complications occurring. Mellor and Ferris15 reviewed 22 De Quervain’s procedures and found that the use of a longitudinal incision was associated with significant risk of complications; of the 17 patients receiving a longitudinal incision, 4 had a poor cosmetic result and 6 exhibited evidence of radial nerve injury. They suggest that avoiding a longitudinal incision may decrease incidence of these postoperative complications.15 Alexander et al.16 developed the EPB entrapment test, which is a simple test based on pain with resisted movement to identify patients preoperatively with a higher likelihood of having their EBP tendon contained within its own subsheath. The test showed 81% specificity and 50% sensitivity for determining the presence preoperatively of a separate EBP sheath.16 While the surgeon should always examine the compartment intraoperatively for the presence of subsheaths, positive findings on the EPB entrapment test can alert surgeons preoperatively to pay particular attention for this finding.
Nothing to disclose.
Citations
- Walker-Bone K, Palmer KT, Reading I, Coggon D, Cooper C. Prevalence and impact of musculoskeletal disorders of the upper limb in the general population. Arthritis Rheum. 2004;51(4):642-651. doi:10.1002/art.20535.
- Rettig AC. Athletic injuries of the wrist and hand: part II: overuse injuries of the wrist and traumatic injuries to the hand. Am J Sports Med. 2004;32(1):262-273. doi:10.1177/0363546503261422.
- Skoff HD. "Postpartum/newborn" de Quervain's tenosynovitis of the wrist. Am J Orthop (Belle Mead NJ). 2001;30(5):428-430.
- Palmer K, Walker-Bone K, Linaker C, et al. The Southampton examination schedule for the diagnosis of musculoskeletal disorders of the upper limb. Ann Rheum Dis. 2000;59(1):5-11. doi:10.1136/ard.59.1.5.
- Clarke MT, Lyall HA, Grant JW, Matthewson MH. The histopathology of de Quervain's disease. J Hand Surg Br. 1998;23(6):732-734. doi:10.1016%2FS0266-7681%2898%2980085-5.
- Moore JS. De Quervain's tenosynovitis: stenosing tenosynovitis of the first dorsal compartment. J Occup Environ Med. 1997;39(10):990-1002. doi:10.1097%2F00043764-199710000-00011.
- Harvey FJ, Harvey PM, Horsley MW. De Quervain's disease: surgical or nonsurgical treatment. J Hand Surg Am. 1990;15(1):83-87. doi:10.1016/S0363-5023(09)91110-8.
- Peters-Veluthamaningal C, Winters JC, Groenier KH, Meyboom-deJong B. Randomised controlled trial of local corticosteroid injections for de Quervain's tenosynovitis in general practice. BMC Musculoskelet Disord. 2009;10:131. doi:10.1186/1471-2474-10-131.
- Witt J, Pess G, Gelberman RH. Treatment of de Quervain tenosynovitis. A prospective study of the results of injection of steroids and immobilization in a splint. J Bone Joint Surg Am. 1991;73(2):219-222. doi:10.2106/00004623-199173020-00010.
- Diop AN, Ba-Diop S, Sane JC, et al. Apport de l'échographie dans la prise en charge de la ténosynovite de de Quervain : à propos de 22 cas. J Radiol. 2008;89(9 pt 1):1081-1084. doi:10.1016/S0221-0363(08)73912-X.
- Chang CY, Kheterpal AB, Vincentini JRT, Huang AJ. Variations of anatomy on MRI of the first extensor compartment of the wrist and association with DeQuervain tenosynovitis. Skeletal Radiol. 2017;46(8):1047-1056. doi:10.1007/s00256-017-2639-0.
- Scheller A, Schuh R, Hönle W, Schuh A. Long-term results of surgical release of de Quervain's stenosing tenosynovitis. Int Orthop. 2009;33(5):1301-1303. doi:10.1007/s00264-008-0667-z.
- Ta KT, Eidelman D, Thomson JG. Patient satisfaction and outcomes of surgery for de Quervain's tenosynovitis. J Hand Surg Am. 1999;24(5):1071-1077. doi:10.1053/jhsu.1999.1071.
- Rogozinski B, Lourie GM. Dissatisfaction after first dorsal compartment release for de Quervain tendinopathy. J Hand Surg Am. 2016;41(1):117-119. doi:10.1016/j.jhsa.2015.09.003.
- Mellor SJ, Ferris BD. Complications of a simple procedure: de Quervain's disease revisited. Int J Clin Pract. 2000;54(2):76-77.
- Alexander RD, Catalano LW, Barron OA, Glickel SZ. The extensor pollicis brevis entrapment test in the treatment of de Quervain's disease. J Hand Surg Am. 2002;27(5):813-816. doi:10.1053/jhsu.2002.35309.
Cite this article
Kalbian I, Ilyas AM. De Quervain's release (cadaver). J Med Insight. 2022;2022(206.3). doi:10.24296/jomi/206.3.