Laparoscopic Paraesophageal Hernia Repair
Main Text
Table of Contents
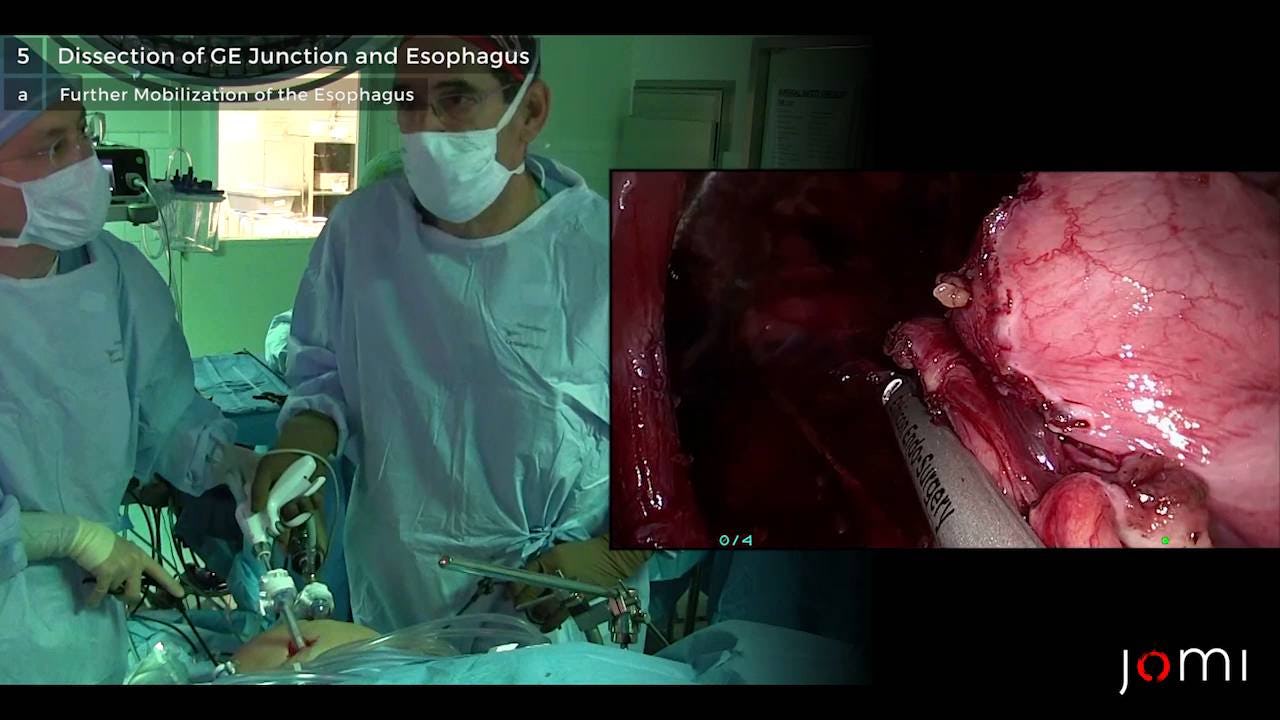
Surgical repair should be considered in all symptomatic paraesophageal hernias. Laparoscopic repair is considered the gold standard with a quicker recovery and lower morbidity and mortality compared to open repairs. The patient in this case presented with worsening dysphagia to solids and dyspnea in the setting of an enlarging paraesophageal hernia with a component of organoaxial volvulus. She underwent a laparoscopic paraesophageal hernia repair with a Toupet fundoplication and posterior gastropexy. The patient exhibited subjective improvement in her dysphagia to solids and dyspnea with exertion as well as an objective improvement in her pulmonary function tests postoperatively.
A true type II paraesophageal hernia is characterized by herniation of the stomach into the posterior mediastinum while maintaining normal positioning of the LES. Mixed hernias (type III) and giant hernias (type IV) are often described as paraesophageal hernias as well. Many of these patients are elderly and are often asymptomatic with their hiatal hernias discovered incidentally on imaging. Symptoms may be caused by gastric outlet obstruction (eg, postprandial pain and early satiety), gastroesophageal reflux, or mechanical trauma to the gastric mucosa (eg, occult blood loss). All symptomatic patients who are good operative candidates should have their paraesophageal hernias repaired. Asymptomatic patients should be observed whereas minimally symptomatic patients who are higher risk surgical candidates require thoughtful decision making before being recommended surgical repair.
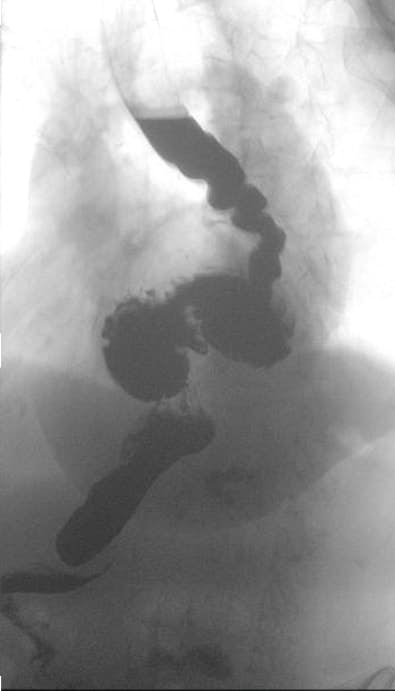
The patient is an 85-year-old woman with a history of GERD and long-standing dysphagia that had recently progressed with associated weight loss. She endorsed significant trouble swallowing solid foods and occasionally even liquids. She also endorsed a history of worsening dyspnea, particularly with activity. She had a known hiatal hernia that was documented to have enlarged on a recent barium swallow. The most recent barium swallow demonstrated weak esophageal peristalsis with a corkscrew shaped esophagus and a large hiatal hernia with organoaxial volvulus. An upper endoscopy confirmed the presence of these anatomical findings as well as the presence of Cameron ulcers. Esophageal motility disclosed a normal LES resting pressure and incomplete LES relaxation on 5 of 11 swallows. Finally, a 24-hour pH impedance study on PPI therapy showed mild reflux but no correlation with symptoms. Her dysphagia did not improve with Botox injections.
On examination, the patient exhibited no abnormal cardiopulmonary findings. She had no prior history of abdominal surgery, and her abdominal exam was normal. Generally, these patients tend to be elderly and require a perioperative cardiopulmonary risk assessment and testing on an individual basis. Obese patients may benefit from a diet and exercise program prior to surgical repair. In the case of this patient, she had no significant cardiac history or history of arrhythmias and a preoperative ECG was unremarkable. Pulmonary function testing was performed given her worsening dyspnea. She was found to have a moderate restrictive defect without significant improvement with albuterol administration. Her worsening dyspnea was thought to be related to her enlarging paraesophageal hernia.
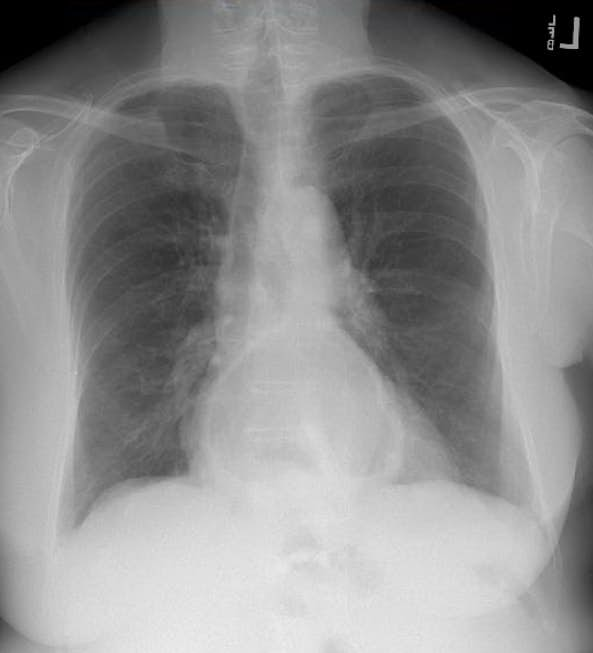
Initial diagnosis is most often made incidentally either on a chest radiograph demonstrating an air-fluid level in the mediastinum posterior to the heart, on a CT scan ordered for other symptoms, or during an upper GI endoscopy. For surgical candidates, evaluation consists of assessing the patient’s overall health status as well as defining the anatomy. CT provides the benefit of three-dimensional anatomy of the hernia. Patients who have a component of preoperative dysphagia should undergo esophageal manometry prior to any fundoplication. An upper endoscopy must be performed preoperatively to exclude concomitant disease such as Barrett’s esophagus, peptic ulcer disease, neoplasms, or other pathology.
Paraesophageal hernias are a disease of the elderly with a median age of presentation between 60-70 years old. Paraesophageal hernias represent a small subset of hiatal hernias (5-10%) and can range from asymptomatic to life-threatening complications. Most of these hernias are asymptomatic or minimally symptomatic, but a small subset of patients can progress to developing acute symptoms, estimated to be about 1% risk of symptom progression per year.1
For symptomatic patients, there are three primary approaches: 1) an open transabdominal approach through an upper midline laparotomy, 2) an open transthoracic approach through a left thoracotomy, and 3) a laparoscopic approach. Laparoscopic repair is considered the standard of care with lower overall morbidity and mortality compared to open repair. The principles of the repair are the same irrespective of access: reduction of intra-abdominal contents, dissection and removal of the hernia sac, mobilization and tension-free return of the gastroesophageal junction into the abdomen, and repair of the diaphragmatic defect. The addition of an anti-reflux procedure or fundoplication should be considered in all patients to minimize post-op reflux symptoms. If dysmotility is present, a partial fundoplication is preferred.
Surgical repair is indicated to relieve symptoms. In patients with minimal symptoms, the risk of complications from surgery must be weighed against the lifetime risk of strangulation or progression of symptoms. This risk is about 1-2% annually.
Our patient presented with reflux and weight loss in the setting of progressive dysphagia. Her evaluation disclosed concomitant esophageal dysmotility and gastroesophageal junction obstruction (as well as worsening dyspnea) thought to be due to her large paraesophageal hernia. We elected to proceed with a laparoscopic paraesophageal hernia repair with a partial fundoplication, expecting her dysphagia to improve with restoration of more normal anatomy.
The vast majority of paraesophageal hernias can be repaired laparoscopically. However, surgeons performing these procedures must be prepared for difficult cases wherein esophageal lengthening or adjunctive techniques for crural repair are needed. Patient factors such as obesity, hepatomegaly, or extensive prior abdominal surgery may alter surgical plans, and patients with BMI’s > 35 should generally not be offered elective surgical paraesophageal hernia repair. The use of mesh to reinforce repairs is controversial with no high-level evidence to suggest that absorbable mesh improves long-term outcomes. Prior to proceeding with repair, it is important to weigh the morbidity and mortality of elective repair compared to the lifetime risk of volvulus and need for an emergent surgery and its associated risks.
FINAL PATHOLOGIC DIAGNOSIS:
A. LIVER MASS EXCISION:
Cavernous hemangioma with infarction and sclerosis. There is no evidence of malignancy.
CLINICAL HISTORY:
Paraesophageal hernia, incidentally found liver mass.
SPECIMENS SUBMITTED:
A. LIVER MASS EXCISION
GROSS DESCRIPTION:
A. Received fresh labeled "liver mass," is a 2.7 x 2.6 x 1.8 cm, firm, predominantly thinly encapsulated pink-tan tissue. The cauterized resection margin is inked blue, and the remainder of the specimen is inked black. The specimen is serially sectioned to reveal a mottled tan-white to pink-tan solid cut surface with scattered punctate areas of hemorrhage. The specimen is entirely submitted in cassettes A1-A6.
Hiatal hernia was first described in the 16th century and most notably published by Bowditch in 1853 in a review of post-mortem findings from previously published cases.1 With the advent of radiography and x-rays, hiatal hernias were first diagnosed in living patients in the early 20th century. It was also at this time that Akerlund described paraesophageal hernias and attempted to classify hiatal hernias.1 Soresi described the first transabdominal approach to repair in 1919 while the earliest series of elective repair was described by Harrington in 1928 at the Mayo Clinic.1 In 1950, Sweet first published his transthoracic approach to paraesophageal hernia repair at the Massachusetts General Hospital.1 With the advent of minimally invasive surgery, the first laparoscopic paraesophageal hernia repair was described in 1992 and is now often described as the standard of care.
Hiatal hernias occur when a portion of the normally intra-abdominal stomach prolapses into the posterior mediastinum through the diaphragmatic hiatus.2 The most common type of hiatal hernia is the type I or sliding hernia, in which the gastroesophageal junction (GEJ) migrates through the diaphragmatic hiatus, thus displacing the location of the lower esophageal sphincter (LES) and exposing the LES to negative intrathoracic pressure. This combination of reduced pressure in the LES and displacement of its normal anatomical position leads to disruption of the anti-reflux mechanism of the LES.2 A true paraesophageal hernia (type II), while rare, is described as an upward herniation of the fundus of the stomach with a normally positioned GEJ. The term paraesophageal hernias is also used to describe both type III hiatal hernias where both the GEJ and fundus of the stomach are intrathoracic and type IV or giant paraesophageal hernias where additional intra-abdominal organs are herniated through the diaphragmatic hiatus as well.
Most hiatal hernias are seen in the elderly with the suggested pathophysiology that increasing age predisposes to changes and weakening of the crural muscles and surrounding connective tissue that make up the hiatal hernia margins. The large majority are asymptomatic and discovered incidentally on imaging or upper endoscopy. However, symptoms can range from mild in severity, such as gastroesophageal reflux and vague epigastric pain, to more severe, such as bleeding with chronic anemia, impaired pulmonary function and life-threatening organoaxial volvulus.
Historically, there was a general agreement amongst surgeons that all symptomatic paraesophageal hernias should be repaired in patients without substantial operative risk. The repair of asymptomatic paraesophageal hernias is more controversial. Initially, surgical repair, regardless of symptoms, was favored due to the fear of life-threatening organoaxial volvulus, once estimated to have a mortality as high as 30% by Skinner and Belsey in 1967 and 56% by Hill in 1973.3,4 These numbers overestimate the true mortality of emergency surgery for gastric volvulus. An analysis of the American College of Surgeons National Surgical Quality Improvement Program (NSQIP) database demonstrated that paraesophageal hernia repairs performed in an emergency setting had a mortality of 8%, which was 10 times greater than the elective surgery group but far lower than previous estimates.5 With multivariable analysis controlling for patient and disease-related factors, the study also found that emergent surgery did not independently predict mortality. They concluded that increased mortality was more a function of severe preoperative comorbidities and poor functional status that would have otherwise excluded patients from elective repair.5 Ballian et al developed a predictive model for perioperative mortality, identifying non-elective operation, age 80 or greater, history of pulmonary disease, and history of congestive heart failure as variables that carry increased risk for perioperative mortality.6
Stylopoulos et al challenged the idea that asymptomatic PEH should be repaired to prevent life threatening complications by championing a more conservative approach. Using a Markov Monte Carlo analytic model, the authors tracked a hypothetical cohort of asymptomatic and minimally symptomatic patients and outcomes associated with elective laparoscopic repair and a conservative watchful waiting strategy. If symptom progression is constant and age dependent, then the risk of developing life-threatening symptoms for a 65-year-old patient is 18% or 1.1% per year.7 Assuming a mortality of emergency surgery of 5.4% from pooled data and the Nationwide Inpatient Sample (NIS) database, then the overall risk of death from watchful waiting was approximately 1%, similar to the pooled estimate of 1.38% for elective laparoscopic repair.7 Watchful waiting was the optimal treatment strategy for 83% of patients in the analysis.
Although paraesophageal hernia were initially repaired via an open transabdominal or transthoracic approach, laparoscopic repair has now emerged as the standard for care. Benefits of laparoscopic PEH repair include less postoperative pain, shorter length of stay, faster recovery, and improvement in quality of life.8 Patients undergoing laparoscopic paraesophageal hernia repair also have fewer overall complications, less need for intensive care unit care, and fewer 30-day readmissions in addition to the aforementioned benefits.9 Mungo et al examined the NSQIP database including 8186 patients who had undergone a PEH (laparoscopic vs open) and discovered an overall 30-day mortality of 0.92% (2.6% open, 0.5% laparoscopic) with significantly lower morbidity in laparoscopic repair, even after adjusted for emergent cases.10 Fullem et al echoed these findings after examining the NIS database (23,514 patients) and concluded that laparoscopic repair is associated with lower mortality compared to an open approach in uncomplicated PEH repair (0.57% vs 1.34%).11
The addition of a fundoplication following repair helps minimize post-op reflux symptoms. Even though reduction of the hernia and mobilization of the stomach to a normal anatomic position alone significantly reduces reflux symptoms (54.6% to 18.2%, P = 0.011), the addition of a fundoplication shows an even more substantial reduction in these symptoms (67.7% to 5.4%, P < 0.001).12 Fundoplication has no impact on reducing hernia recurrence even though it has been postulated that the wrap helps anchor the stomach within the abdomen. Fundoplication should be avoided in patients with preoperative dysphagia or abnormal manometry suggestive of esophageal dysmotility.
Paraesophageal hernia repair provides nearly two-thirds of patients with complete symptom relief and significantly improves quality of life.13 Lidor et al found significant improvement in quality of life scores following surgical repair. All individual symptoms improved significantly except early satiety, nausea, pain with swallowing, and bloating/gas at 36 months.14 These symptoms still demonstrated improvement though they were not statistically significant. Almost all patients with postoperative heartburn symptoms are easily controlled with PPI therapy and very rarely require re-operation.
The downside of laparoscopic repair compared to an open approach is a higher rate of radiographic recurrence. It is thought that open surgery facilitates development of adhesions which can anchor the stomach in an intra-abdominal position. Laparoscopic repair has an estimated radiographic recurrence of about 27% at 1 year, but very rarely are these recurrences symptomatic and require re-operation.14 Some studies have suggested that the addition of a gastropexy helps reduce recurrence rates, but the evidence is mixed.14-16 A meta-analysis of laparoscopic mesh repairs demonstrated improved hernia recurrence rates compared to primary repair (12.1% vs 20.5%).17 Even when restricted to studies with at least 2 years follow-up, there was a decreased recurrence rate (11.5% vs 25.4%).17 However, not all studies were able to replicate the finding that repair with biologic mesh reduces long term recurrence. Oelschlager et al found that recurrence rates at 6 months were lower in the mesh group but there was no difference between biologic mesh repair and primary crural repair at 5 years.18 The use of mesh and the safety of its use has also been a subject of debate. An analysis of the NSQIP database found no statistically significant difference in 30-day mortality or secondary morbidity in laparoscopic repairs with and without mesh placement.19 Mesh repair should be considered when the crural muscles are too attenuated for primary repair.
We used standard laparoscopic equipment with non-absorbable mesh available.
We have nothing to disclose.
The patient referred to in this video article has given their informed consent to be filmed and is aware that information and images will be published online.
Citations
- Stylopoulos N, Rattner DW. The history of hiatal hernia surgery: from Bowditch to laparoscopy. Ann Surg. 2005;241(1):185-193. doi:10.1097/01.sla.0000149430.83220.7f.
- Maziak DE, Pearson FG. Massive (paraesophageal) hiatal hernia. In: Patterson GA, Cooper JD, Deslauriers J, et al, eds. Pearson's Thoracic and Esophageal Surgery. 3rd ed. Philadelphia, PA: Churchill Livingstone; 2008:233-238.
- Skinner DB, Belsey RH. Surgical management of esophageal reflux and hiatus hernia. Long-term results with 1,030 patients. J Thorac Cardiovasc Surg. 1967;53(1):33-54.
- Hill LD. Incarcerated paraesophageal hernia: a surgical emergency. Am J Surg. 1973;126(2):286-291. doi:10.1016/S0002-9610(73)80165-5.
- Augustin T, Schneider E, Alaedeen D, et al. Emergent surgery does not independently predict 30-day mortality after paraesophageal hernia repair: results from the ACS NSQIP Database. J Gastrointest Surg. 2015;19(12):2097-2104. doi:10.1007/s11605-015-2968-z.
- Ballian N, Luketich JD, Levy RM, et al. A clinical prediction rule for perioperative mortality and major morbidity after laparoscopic giant paraesophageal hernia repair. J Thorac Cardiovasc Surg. 2013;145(3):721-729. doi:10.1016/j.jtcvs.2012.12.026.
- Stylopoulos N, Gazelle GS, Rattner DW. Paraesophageal hernias: operation or observation? Ann Surg. 2002;236(4):492-501. doi:10.1097/01.SLA.0000029000.06861.17.
- Draaisma WA, Gooszen HG, Tournoij E, Broeders IAMJ. Controversies in paraesophageal hernia repair; a review of literature. Surg Endosc. 2005;19(10):1300-1308. doi:10.1007/s00464-004-2275-3.
- Nguyen NT, Christie C, Masoomi H, Matin T, Laugenour K, Hohmann S. Utilization and outcomes of laparoscopic versus open paraesophageal hernia repair. Am Surg. 2011;77(10):1353-1357. https://www.ingentaconnect.com/content/sesc/tas/2011/00000077/00000010/art00018.
- Mungo B, Molena D, Stem M, Feinberg RL, Lidor AO. Thirty-day outcomes of paraesophageal hernia repair using the NSQIP Database: should laparoscopy be the standard of care? J Am Coll Surg. 2014;219(2):229-236. doi:10.1016/j.jamcollsurg.2014.02.030.
- Fullum TM, Oyetunji TA, Ortega G, et al. Open versus laparoscopic hiatal hernia repair. JSLS. 2013;17(1):23-29. doi:10.4293/108680812X13517013316951.
- van der Westhuizen L, Dunphy KM, Knott B, Carbonell AM, Smith DE, Cobb WS. The need for fundoplication at the time of laparoscopic paraesophageal hernia repair. Am Surg. 2013;79(6):572-577. https://www.ingentaconnect.com/contentone/sesc/tas/2013/00000079/00000006/art00016.
- El Khoury R, Ramirez M, Hungness ES, Soper NJ, Patti MG. Symptom relief after laparoscopic paraesophageal hernia repair without mesh. J Gastrointest Surg. 2015;19(11):1938-1942. doi:10.1007/s11605-015-2904-2.
- Lidor AO, Steele KE, Stem M, Fleming RM, Schweitzer MA, Marohn MR. Long-term quality of life and risk factors for recurrence after laparoscopic repair of paraesophageal hernia. JAMA Surg. 2015;150(5):424-431. doi:10.1001/jamasurg.2015.25.
- Poncet G, Robert M, Roman S, Boulez JC. Laparoscopic repair of large hiatal hernia without prosthetic reinforcement: late results and relevance of anterior gastropexy. J Gastrointest Surg. 2010;14(12):1910-1916. doi:10.1007/s11605-010-1308-6.
- Ponsky J, Rosen M, Fanning A, Malm J. Anterior gastropexy may reduce the recurrence rate after laparoscopic paraesophageal hernia repair. Surg Endosc. 2003;17(7):1036-1041. doi:10.1007/s00464-002-8765-2.
- Müller-Stich BP, Kenngott HG, Gondan M, et al. Use of mesh in laparoscopic paraesophageal hernia repair: a meta-analysis and risk-benefit analysis. PloS One. 2015;10(10):e0139547. doi:10.1371/journal.pone.0139547.
- Oelschlager BK, Pellegrini CA, Hunter J, et al. Biologic prosthesis reduces recurrence after laparoscopic paraesophageal hernia repair: a multicenter, prospective, randomized trial. Ann Surg. 2006;244(4):481-490. doi:10.1097/01.sla.0000237759.42831.03.
- Kubasiak J, Hood KC, Daly S, et al. Improved patient outcomes in paraesophageal hernia repair using a laparoscopic approach: a study of the National Surgical Quality Improvement Program data. Am Surg. 2014;80(9):884-889. https://www.ingentaconnect.com/contentone/sesc/tas/2014/00000080/00000009/art00022.