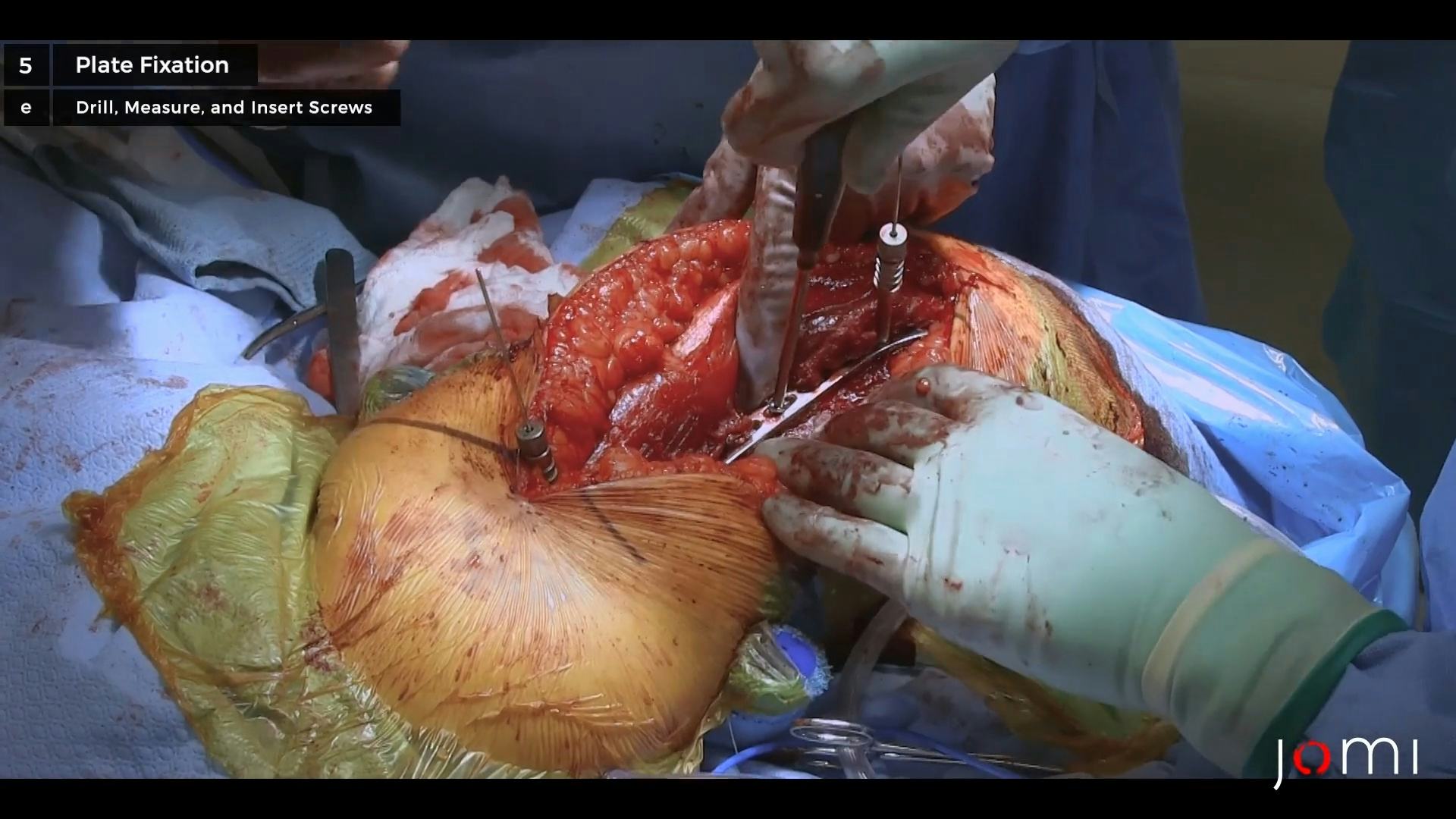
Open Reduction and Internal Fixation of a Diaphyseal Periprosthetic Humeral Fracture
Main Text
Table of Contents
Periprosthetic humeral shaft fractures are increasing in incidence as shoulder replacements become more common. Surgical management of humeral shaft fractures can only be deemed appropriate when the degree of pain, the extent of disability, and the number of comorbid conditions are taken into consideration. Among trauma surgeons there exists no preferred surgical approach to fractures of different segments of the humerus; however, the anterolateral approach to midshaft fractures is the most common although viable alternative approaches exist. In this case, we perform an open reduction and internal fixation of a diaphyseal periprosthetic humeral fracture with a posterior triceps sparing approach.
Humeral shaft fractures are one of the most common fractures of the upper extremity. The anatomy of the radial nerve makes the approaches during open reduction and internal fixation (ORIF) difficult. Although anterolateral approaches are commonly used for proximal and middle third shaft fractures, the posterior approach to the humerus can be used for fractures along the entire diaphyseal humerus. This video outlines the posterior triceps-sparing approach for ORIF of a diaphyseal periprosthetic humeral fracture.
This is a 57-year-old female with a history of failed left total shoulder replacement with a revision to reverse total shoulder replacement, and who sustained a distal third humeral shaft fracture and resulting radial nerve palsy during a recent fall. Of note, the patient has a history notable for ataxia secondary to gentamicin toxicity that causes her to rely significantly on her upper extremities.
Patients with humeral shaft fractures often experience pain, swelling, and weakness of the upper extremity. Patients can also experience shortening of the extremity in varus with some crepitus with the movement of the extremity. It is important to evaluate for compromise of skin integrity as an overlying laceration would be described as an open fracture.1
It is important to confirm the limb is neurovascularly intact distal to the injury as the radial nerve and brachial artery are at high risk. A significant population of those with humeral shaft fractures experience neurovascular complications such as radial nerve palsy. Radial nerve palsy of the middle third of the arm can present as difficulty with the extension of the wrist and digits, as well as supination of the forearm. Radial nerve palsy can also present as numbness over the dorsal aspects of the thumb, index, and middle fingers.1
Evaluation should begin with anteroposterior (AP) and lateral radiographs. Traction view radiographs and CT scans can be helpful for preoperative planning if the extremity is significantly displaced or comminuted.
In this case, radiographs show skeletally mature AP and lateral views with the intact prosthesis and a cement mantle that extends distally. There is a diaphyseal humeral fracture distal to the cement mantle.
If left untreated, the natural history of this patient’s condition is one of increasing pain and disability. The patient would likely have a significant weakness with flexion and extension of the extremity distal to the fracture due to compromise of muscles and neurovascular structures at and around the fracture site. Stiffness and limited range of motion of the extremity would also be likely given the patient’s radial nerve palsy and large body habitus.
The standard of treatment of humeral shaft fractures is nonoperative management with immediate immobilization via coaptation splint, sling, and/or swath followed by functional bracing. Surgical treatment is generally reserved for patients who suffer open fractures, polytrauma, and fail to tolerate or maintain alignment in a functional brace.2 Mainstay of operative management includes ORIF as well as intramedullary nailing of the humerus.2,3
Given the degree of pain and loss of function of the upper extremity, it is evident that nonoperative management of this periprosthetic humeral fracture was not a realistic option. Intramedullary nailing was not a viable option due to the existing prosthesis in the proximal humerus. The goals of treatment were to decrease pain and improve function by providing absolute stability and primary bone healing. Because the prosthesis was intact and without known complications, replacement of the prosthesis with a longer stem was a less desirable treatment strategy. In this case, goals of treatment would be accomplished best by ORIF with lag screws and neutralization plating with a contoured plate since using cerclage wires for fixation around the humerus is challenging and risks injury to many surrounding neurovascular structures in the humerus. Additionally, particularly in this case, it was believed that lag screws offer superior fixation when compared to short locking screws around the cement mantle.4
Historically, disputes existed as to whether radial nerve palsy was an indication for surgery.5-8 However, given that we understand that, in closed fractures, radial nerve injury often is neuropraxia, radial nerve palsy is no longer a clear indication for surgical exploration and ORIF of a closed fracture. Open fractures with associated radial nerve palsy, however, represent radial nerve laceration 60% of the time and are still an indication for surgical exploration of the radial nerve and ORIF of the fracture.1,9,10 Additionally, indications that require ORIF of a fracture include those that otherwise lead to severe debilitation including polytraumas and pathological fractures.
Several approaches to the midshaft humerus exist for the ORIF of fractures. Anterolateral approaches are commonly used, but the posterior approach also offers distinct advantages including the ability for distal exposure extension and biomechanical advantages due to plating on the tension side of the humerus.11,12 Currently, there is no consensus on which approach is preferable for each segment.12
The posterior triceps-sparing approach used in this case allows for several advantages over posterior triceps-splitting approaches. One advantage includes the avoidance of injury to the triceps muscle, which decreases the risk of elbow contracture and postoperative triceps weakness.12 Additionally, the triceps-sparing approach allows for complete visualization of the radial nerve and does not require the use of a tourniquet since the plane of dissection involves few vascular structures.12 Finally, two studies by Schildhauer et al. and Jamali et al. have suggested that this approach decreases operative time in distal humerus fracture.13,14
Although the posterior and posterolateral approaches offer greater visualization of fractures and the radial nerve, one study by Lotzien et al. and a meta-analysis by Saracco et al. demonstrate no significant differences in union rate, postoperative range of motion, or bleeding between anterior and posterior approaches.11,15 Thus, the posterior, triceps-sparing approach used during this case remains appropriate for optimal patient outcomes.
Outcomes of humeral shaft fractures are generally favorable with nearly 90% achieving a satisfactory union.1 The study by Lotzien et al. demonstrates a 98% union rate of the humeral shaft fractures. Furthermore, the rates of the union of periprosthetic humeral fracture with surgical management are favorable with union rates reported above 98%.16,17 Periprosthetic humerus fractures have been reported to take an average of 6.8 months to heal.17
Possible complications of surgery include stiffness, infection, symptomatic hardware, brachial artery injury, radial nerve injury, delayed union, malunion, and nonunion.18,19
Rehabilitation is dependent on the adequacy of fracture fixation. Passive and active-assisted range of motion is permitted at the shoulder and elbow on the first postoperative day. Active range of motion can begin if there is radiographic evidence of progression of fracture healing at approximately the 6th postoperative week.20, 21 If no signs of radiographic healing, the progression of rehabilitation will be delayed.
- DePuy Synthes 3.5-mm LCP Distal Humerus Plates
- Lag screws
Nothing to disclose.
The patient referred to in this video article has given their informed consent to be filmed and is aware that information and images will be published online.
Citations
- Bounds EJ, Kok SJ. Humeral Shaft Fractures. StatPearls [Internet]. StatPearls Publishing; 2020.
- Walker M, Palumbo B, Badman B, Brooks J, Van Gelderen J, Mighell M. Humeral shaft fractures: a review. J Shoulder Elbow surg. 2011;20(5):833-844. doi:10.1016/j.jse.2010.11.030.
- Clement ND. Management of humeral shaft fractures; non-operative versus operative. Arch Trauma Res. 2015;4(2). doi:10.5812/atr.28013v2.
- Kampshoff J, Stoffel KK, Yates PJ, Erhardt JB, Kuster MS. The treatment of periprosthetic fractures with locking plates: effect of drill and screw type on cement mantles: a biomechanical analysis. Arch Orth Trauma Surg. 2010;130(5):627-632. doi:10.1007/s00402-009-0952-3.
- Vansteenkiste FP, Rommens PM, Broos PL. [Is a radial nerve paralysis in a humeral shaft fracture an indication for surgery? Indications]. Acta Chir Belg. Jul-Aug 1989;89(4):215-20. Is een nervus radialis paralyse bij een humerus schaft fractuur een indicatie tot operatie? Indications.
- Holstein A, Lewis G. Fractures of the humerus with radial-nerve paralysis. J Bone Joint Surg Am. 1963;45(7):1382-1388.
- Kettelkamp DB, Alexander H. Clinical review of radial nerve injury. J Trauma Acute Care Surg. 1967;7(3):424-432. doi:10.1097/00005373-196705000-00007.
- Ekholm R, Ponzer S, Törnkvist H, Adami J, Tidermark J. Primary radial nerve palsy in patients with acute humeral shaft fractures. J Orth trauma. 2008;22(6):408-414. doi:10.1097/BOT.0b013e318177eb06.
- Laulan J. High radial nerve palsy. Hand Surg and Rehab. 2019;38(1):2-13. doi:10.1016/j.hansur.2018.10.243.
- Agarwal A, Chandra A, Jaipal U, Saini N. A panorama of radial nerve pathologies-an imaging diagnosis: a step ahead. Ins Imag. 2018;9(6):1021-1034. doi:10.1007/s13244-018-0662-x.
- Lotzien S, Hoberg C, Rausch V, Rosteius T, Schildhauer TA, Gessmann J. Open reduction and internal fixation of humeral midshaft fractures: anterior versus posterior plate fixation. BMC Musc dis. 2019;20(1):527. doi:10.1186/s12891-019-2888-2.
- Zlotolow DA, Catalano III LW, Barron AO, Glickel SZ. Surgical exposures of the humerus. JAAOS. 2006;14(13):754-765. doi:10.5435/00124635-200612000-00007.
- Schildhauer TA, Nork SE, Mills WJ, Henley MB. Extensor mechanism-sparing paratricipital posterior approach to the distal humerus. J Ortho Trauma. 2003;17(5):374-378. doi:10.1097/00005131-200305000-00009.
- Jamali A, Mehboob G, Ahmed S. Extensor mechanism sparing approach to the elbow for reduction and internal fixation of intercondylar fracture of the humerus. J Pak Med Assoc. 1999;49(7):164-7.
- Saracco M, Smimmo A, De Marco D, et al. Surgical approach for fracture of distal humerus: posterior vs lateral. Ortho Rev. 2020;12(s1). https://doi.org/10.4081/or.2020.8664.
- Groh GI, Heckman MM, Wirth MA, Curtis RJ, Rockwood CA Jr. Treatment of fractures adjacent to humeral prostheses. J Shoulder Elbow Surg. 2008;17(1):85-89. doi:10.1016/j.jse.2007.05.007.
- Andersen JR, Williams CD, Cain R, Mighell M, Frankle M. Surgically treated humeral shaft fractures following shoulder arthroplasty. JBJS. 2013;95(1):9-18. doi:10.2106/JBJS.K.00863.
- Zarkadis NJ, Eisenstein ED, Kusnezov NA, Dunn JC, Blair JA. Open reduction–internal fixation versus intramedullary nailing for humeral shaft fractures: an expected value decision analysis. J Shoulder Elbow Surg. 2018;27(2):204-210. doi:10.1016/j.jse.2017.08.004.
- Gottschalk MB, Carpenter W, Hiza E, Reisman W, Roberson J. Humeral shaft fracture fixation: incidence rates and complications as reported by American Board of Orthopaedic Surgery part II candidates. JBJS. 2016;98(17):e71. doi:10.2106/JBJS.15.01049.
- Steinmann SP, Cheung EV. Treatment of periprosthetic humerus fractures associated with shoulder arthroplasty. JAAOS. 2008;16(4):199-207. doi:10.5435/00124635-200804000-00003.
- Seitz WH Jr. Periprosthetic fractures: repair, revise, or treat conservatively. Elsevier. 2017:153-158. doi:10.1053/j.sart.2017.12.013.
Cite this article
Amakiri IC, Weaver MJ. Open reduction and internal fixation of a diaphyseal periprosthetic humeral fracture. J Med Insight. 2023;2023(119). doi:10.24296/jomi/119.